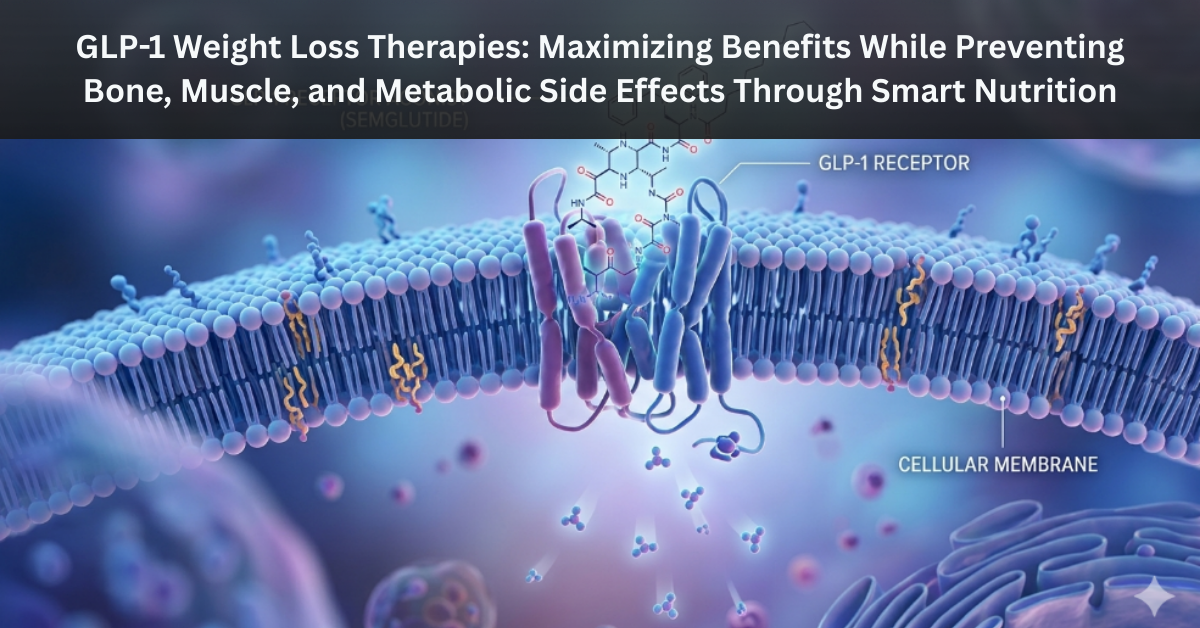
Introduction: A Breakthrough with a Caution
GLP-1 receptor agonists such as semaglutide and liraglutide have transformed the treatment of obesity and type-2 diabetes. These medications reduce appetite, slow gastric emptying, and improve insulin regulation, enabling substantial weight loss and metabolic improvements. Millions of patients worldwide are now using them to manage obesity, diabetes, and metabolic syndrome.
However, as the use of GLP-1 therapies expands, new research is highlighting an important reality: rapid pharmacologically induced weight loss may come with unintended physiological consequences if nutrition and lifestyle are neglected.
Recent research presented at the American Academy of Orthopaedic Surgeons analyzed data from nearly 150,000 patients and found that GLP-1 users had higher long-term risks of certain musculoskeletal conditions. Over five years, osteoporosis risk was about 30% higher, gout risk increased 12%, and osteomalacia occurred more frequently among users compared with non-users.
These findings do not mean GLP-1 drugs are unsafe. In fact, their benefits in diabetes control, cardiovascular risk reduction, and obesity management remain substantial. But the emerging evidence suggests that GLP-1 therapy should not be viewed as a standalone solution. Instead, it works best when integrated with a personalized diet, targeted micronutrients, adequate protein intake, and musculoskeletal protection strategies.
This blog explores how a nutritionally optimized GLP-1 program can help patients maximize metabolic benefits while minimizing long-term complications.
Why Side Effects May Occur During GLP-1 Therapy
GLP-1 drugs primarily act by suppressing appetite and slowing digestion. While this helps reduce caloric intake, it can also inadvertently reduce intake of essential nutrients such as protein, calcium, vitamin D, and micronutrients.
Three major mechanisms explain potential side effects.
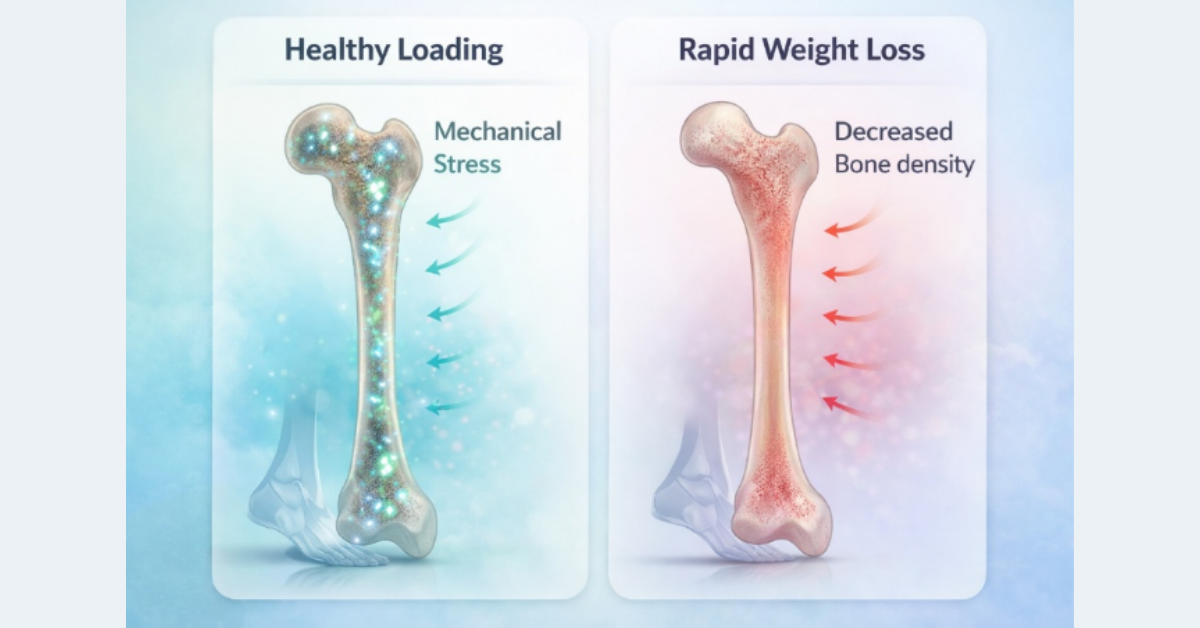
- Rapid Weight Loss Reduces Mechanical Bone Loading
Bones respond to mechanical stress. When body weight decreases rapidly, skeletal loading decreases as well, which can reduce bone density over time.
- Reduced Nutrient Intake
Because appetite is suppressed, patients may unintentionally consume insufficient:
- Protein
- Calcium
- Vitamin D
- Magnesium
- B vitamins
Studies show that 14% of GLP-1 users develop vitamin D deficiency within one year, highlighting the importance of nutritional monitoring.
- Lean Muscle Loss
Rapid weight loss may lead to 15–25% reduction in lean muscle mass, especially if protein intake and resistance training are inadequate.
Muscle loss indirectly weakens bone strength because muscle contraction stimulates bone formation.
Expert Insights from Indian Clinicians
To better understand how clinicians view this issue in India, we gathered insights from specialists.
Dr. Prasanna, Orthopedic Surgeon, Bangalore
“GLP-1 medications are powerful tools for obesity and diabetes, but bone health must be monitored. When patients lose weight rapidly without adequate protein, calcium and vitamin D, the musculoskeletal system becomes vulnerable. Nutritional support and resistance exercise are essential companions to these therapies.”
Dr. Venkata Ramana, Endocrinologist, Hyderabad
“GLP-1 therapy improves metabolic health dramatically, but appetite suppression can lead to hidden nutrient deficiencies. Personalized diet plans and micronutrient supplementation are critical for sustaining long-term metabolic outcomes.”
Dr. Aziz Khan, Internal Medicine Specialist, Chennai
“Patients often assume the drug alone will solve obesity. In reality, the best outcomes occur when GLP-1 therapy is integrated with lifestyle medicine—adequate protein intake, micronutrients, gut health optimization, and physical activity.”
Common Side Effects Linked with GLP-1 Therapy
Side Effect | Possible Cause | Prevention Strategy |
Bone density reduction | Reduced calcium, vitamin D, mechanical load | Calcium regulators, vitamin D3, resistance exercise |
Muscle loss | Low protein intake | 1.2–1.5 g/kg protein |
Gout | Rapid fat loss increasing uric acid | Hydration, uric acid control diet |
Fatigue | micronutrient deficiency | B-vitamins, magnesium |
Hair loss | rapid metabolic shift | protein, iron, biotin |
Osteomalacia | mineral deficiency | vitamin D3 + calcium |
Who Is Most Likely to Experience GLP-1 Side Effects?
Certain individuals are more vulnerable to nutritional complications.
High Risk Groups
Population | Reason |
Post-menopausal women | higher baseline osteoporosis risk |
Elderly patients | reduced bone remodeling capacity |
Very low calorie eaters | severe nutrient deficiency |
Rapid weight loss (>10% body weight in 3 months) | metabolic stress |
Sedentary individuals | lack of bone-strengthening activity |
Patients with diabetes >10 years | poor bone quality |
A Nutritional Strategy to Protect Patients on GLP-1 Therapy
- Adequate Protein Intake
Protein is the most critical nutrient during pharmacological weight loss.
Recommended intake:
1.2–1.5 g protein per kg body weight
Sources
- Whey protein
- Lean fish
- Eggs
- Lentils
- Greek yogurt
Protein prevents muscle loss and supports bone structure.

- Calcium Regulation — Not Just Calcium Intake
Many clinicians focus only on calcium supplementation, but the real goal is calcium regulation and bone remodeling.
Natural regulators include:
Cissus quadrangularis
Vitamin K2
Magnesium
Collagen peptides
Cissus quadrangularis has been used in traditional medicine for bone healing and may enhance osteoblast activity and fracture recovery.
- Liposomal Vitamin D3
Vitamin D deficiency is common among obese individuals and may worsen during GLP-1 therapy due to reduced intake and fat redistribution.
Liposomal vitamin D3 offers advantages:
- higher absorption
- better bioavailability
- lower gastrointestinal irritation
Vitamin D supports
- calcium absorption
- muscle function
- immune health
- Magnesium for Metabolic and Musculoskeletal Health
Magnesium is required for:
- vitamin D activation
- muscle contraction
- insulin signaling
Low magnesium can worsen fatigue and muscle weakness during weight loss.
- Collagen Peptides and Connective Tissue Protection
Collagen peptides support
- joint health
- cartilage integrity
- tendon resilience
Some researchers believe tendon injuries associated with rapid weight loss may partly relate to connective tissue changes.
Recommended Supplement Strategy for GLP-1 Patients
Nutrient | Daily Dose Range | Benefit |
Protein | 1.2–1.5 g/kg | muscle preservation |
Vitamin D3 | 1000–2000 IU | bone metabolism |
Magnesium | 200–400 mg | muscle & nerve function |
Vitamin K2 | 90–120 mcg | calcium regulation |
Cissus quadrangularis | 500–1000 mg | bone strengthening |
Collagen peptides | 5–10 g | tendon and joint support |
Diet Blueprint for GLP-1 Therapy
A balanced dietary plan should emphasize nutrient density rather than calorie restriction alone.
Sample Daily Structure
Breakfast
Greek yogurt with nuts and berries
Mid-morning
Protein smoothie
Lunch
Grilled fish or paneer with vegetables and quinoa
Evening snack
Fruit with seeds
Dinner
Lentil soup with vegetables
Before bed
Collagen peptide drink
This structure ensures adequate protein and micronutrient intake even with reduced appetite.

Lifestyle Strategies That Enhance GLP-1 Outcomes
1 Resistance Training
Weight-bearing exercise stimulates bone remodeling and prevents sarcopenia.
Recommended
3 sessions per week
2 Sun Exposure
Natural vitamin D synthesis improves bone health.
15–20 minutes daily sunlight.
3 Hydration
Adequate hydration reduces gout risk by improving uric acid clearance.
4 Sleep Optimization
Sleep regulates appetite hormones and metabolic recovery.
Future of GLP-1 Therapy: Integrated Metabolic Care
Experts increasingly believe GLP-1 therapy will evolve into multimodal metabolic programs combining:
- pharmacotherapy
- personalized nutrition
- nutraceutical support
- lifestyle medicine
Research already shows that combining GLP-1 therapy with healthy lifestyle habits significantly reduces cardiovascular risk compared with medication alone.
The next decade will likely see more integration between endocrinology, nutrition science, and orthopedic health.
Conclusion
GLP-1 medications represent one of the most powerful breakthroughs in metabolic medicine. They have helped millions of patients control diabetes, lose weight, and improve cardiovascular health.
However, like all powerful therapies, they must be used wisely.
The emerging evidence on bone health, gout risk, and nutrient deficiencies should not discourage patients from using GLP-1 drugs. Instead, it highlights the need for a holistic treatment approach.
When combined with:
- personalized diet planning
- adequate protein intake
- targeted micronutrients
- natural calcium regulators like Cissus quadrangularis
- liposomal vitamin D3
- resistance exercise
GLP-1 therapy can deliver its full benefits while minimizing long-term complications.
As Dr. Prasanna summarizes:
“GLP-1 therapy should not replace lifestyle medicine — it should work alongside it.”
Frequently Asked Questions
Not directly, but rapid weight loss and nutrient deficiencies may increase bone risk.
Rapid fat loss can temporarily increase uric acid levels.
Yes. It prevents muscle loss and supports metabolic function.
Typically 1.2–1.5 g/kg body weight.
Many clinicians recommend monitoring vitamin D levels and supplementing when necessary.
Fat tissue stores vitamin D, reducing circulating levels.
No. Calcium regulation also requires vitamin D, magnesium, and vitamin K2.
A medicinal plant traditionally used to support bone healing.
Yes, especially during rapid weight loss without adequate protein intake.
Protein intake and resistance exercise.
Yes, but bone health monitoring is recommended.
High-risk patients may benefit from periodic DEXA scans.
Yes. It significantly improves blood sugar control and reduces cardiovascular risk.
A high-protein, nutrient-dense diet.
Targeted supplementation can help prevent deficiencies.
Collagen supports joint and connective tissue health.
Yes, if nutrient intake and physical activity are inadequate.
It may improve absorption in some individuals.
Yes. Resistance exercise is strongly recommended.
Under medical supervision with nutritional support.