Persistent fatigue, muscle pain, reduced stamina, poor recovery after illness, brain fog, and unexplained joint discomfort are among the most common complaints seen in outpatient practice today. Yet in a large number of cases, routine laboratory reports appear “normal.” This mismatch between symptoms and laboratory findings often reflects functional micronutrient deficiencies—a growing but under-recognized clinical issue in preventive and integrative medicine.
Across India, deficiencies of vitamin B12, vitamin D, ferritin (iron stores), and magnesium are increasingly being identified not only in elderly populations but also among working professionals, students, athletes, and individuals with sedentary lifestyles. These deficiencies affect mitochondrial energy production, neuromuscular signaling, immune regulation, and inflammatory balance long before overt disease develops.
Understanding these hidden deficiencies early can significantly improve long-term metabolic resilience and reduce progression toward chronic disorders.

The Epidemiology of Hidden Micronutrient Deficiencies in India
Recent epidemiological data highlight the scale of this issue:
- Vitamin D deficiency affects 70–90% of urban Indians despite adequate sunlight exposure
• Up to 47% of adults have borderline or low vitamin B12 levels
• Nearly 50–60% of Indian women have low ferritin even without anemia
• Subclinical magnesium deficiency is estimated to affect over 40% of adults, particularly those with stress, diabetes risk, or poor sleep patterns
These deficiencies frequently remain undiagnosed because laboratory reference ranges reflect population averages, not optimal physiological requirements.
Why “Normal Reports” Do Not Always Mean Normal Physiology
Laboratory ranges define disease thresholds—not performance thresholds.
For example:
Vitamin B12 above 200 pg/ml is technically normal
But neurological efficiency often requires >400 pg/ml
Vitamin D above 20 ng/ml prevents rickets
But metabolic and immune stability typically requires >40 ng/ml
Ferritin above 15 ng/ml avoids anemia
But fatigue resistance often improves above 50 ng/ml
Magnesium within reference range may still be insufficient intracellularly
This explains why many individuals continue to experience symptoms despite “normal” reports.

Symptoms Suggesting Functional Micronutrient Deficiency
Common early indicators include:
- persistent fatigue despite adequate sleep
- morning stiffness or muscle tightness
hair fall - brain fog or reduced concentration
- physiotherapy response
- frequent infections
- reduced exercise tolerance
- tingling or numbness
- poor stress resilience
These symptoms often precede detectable biochemical deficiency.
Case Studies from Clinical Practice
(Shared by Dr. Venkatramana, Consultant Physician, Bangalore)
Case Study 1: Persistent Fatigue in a Working Professional
A 38-year-old software professional presented with chronic fatigue despite normal thyroid and hemoglobin reports. Further evaluation showed vitamin B12 at 280 pg/ml and vitamin D at 24 ng/ml. After correction using bioavailable supplementation over three months, energy levels improved significantly and sleep quality normalized.
Case Study 2: Knee Pain with Normal Imaging
A 52-year-old female reported early knee pain without radiological osteoarthritis. Ferritin was 22 ng/ml and vitamin D was 19 ng/ml. After targeted supplementation, pain reduced substantially within 10 weeks without requiring analgesics.
Case Study 3: Slow Recovery After Viral Illness
A 45-year-old male experienced prolonged fatigue after viral infection. Magnesium and vitamin D levels were low-normal. Supplementation improved muscle recovery and exercise tolerance within 8 weeks.
Case Study 4: Recurrent Hair Fall with Borderline Labs
A 29-year-old woman with recurrent hair fall had ferritin 28 ng/ml and B12 310 pg/ml. Correction restored hair density and reduced fatigue within three months.
Which Deficiencies Can Be Safely Corrected with Self-Initiated Supplementation?
Many early-stage deficiencies fall into the preventable and correctable category when identified early.
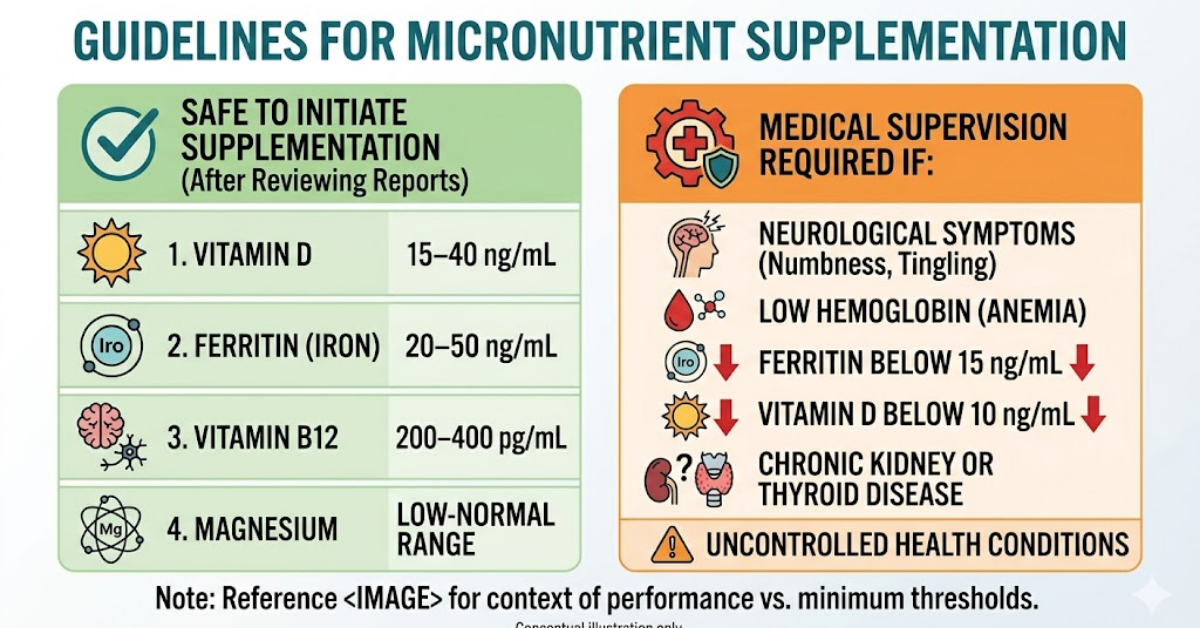
Safe to begin supplementation (after reviewing reports):
- Vitamin D between 15–40 ng/ml
- Ferritin between 20–50 ng/ml
- Vitamin B12 between 200–400 pg/ml
- Magnesium low-normal range
However, medical supervision is required if:
- persistent neurological symptoms are present
- hemoglobin is low
- ferritin below 15
- vitamin D below 10
- chronic kidney disease exists
- thyroid disease is uncontrolled
Recommended Duration of Supplementation (with clinical positioning)
Most micronutrient correction protocols require at least 8–12 weeks to achieve measurable biochemical and symptomatic improvement.
Typical correction windows include:
- Vitamin D: 8–16 weeks
- Vitamin B12: 6–12 weeks
- Ferritin: 12 weeks or longer
- Magnesium: 6–8 weeks
Clinical improvement often begins before laboratory normalization is complete, particularly when absorption-enhanced formulations are used.
In individuals with fatigue, musculoskeletal discomfort, or metabolic stress patterns, clinicians increasingly prefer bioavailable delivery formats such as liposomal vitamin D3–magnesium combinations, liposomal ferric pyrophosphate, or methylated B-vitamin complexes, which may support faster intracellular restoration compared to conventional salts.
Which Deficiencies Can Be Safely Corrected with Self-Initiated Supplementation?
Many early-stage deficiencies fall within the preventable correction window, especially when symptoms are mild and laboratory values remain within borderline ranges.
Examples include:
- Vitamin D between 15–40 ng/ml
- Ferritin between 20–50 ng/ml
- Vitamin B12 between 200–400 pg/ml
- Magnesium in the low-normal range
In such situations, short-term structured supplementation using well-tolerated, absorption-optimized formulations—such as liposomal magnesium–vitamin D combinations or gentle ferric pyrophosphate–based iron preparations—may help restore levels efficiently while minimizing gastrointestinal intolerance.
Medical supervision is recommended if symptoms persist despite correction attempts.
What Should Be Done After Completing a 3-Month Course?
After completing a structured supplementation phase:
- repeat laboratory testing
- review symptom improvement
- adjust maintenance dosing if required
- transition toward dietary reinforcement
Maintenance supplementation is often useful in individuals with:
- vegetarian dietary patterns
- low sunlight exposure
- recurrent fatigue
- metabolic syndrome risk
- heavy menstrual blood loss
Where long-term correction is needed, clinicians may consider lower-dose maintenance strategies using bioavailable micronutrient formats such as liposomal magnesium–vitamin D3 combinations or methylated B-vitamin support, particularly in individuals with persistent absorption variability.
What If Values Do Not Improve After Supplementation?
If laboratory values remain suboptimal after 8–12 weeks of supplementation, several factors should be considered:
- poor gastrointestinal absorption
- chronic inflammation
- thyroid imbalance
- stress-related magnesium depletion
- functional B-vitamin utilization defects
In such cases, switching to absorption-enhanced delivery systems such as liposomal minerals or methylated vitamin formats may improve correction response.
For example:
liposomal ferric pyrophosphate may improve iron tolerability and uptake
liposomal magnesium–vitamin D3 combinations may support neuromuscular recovery
methylcobalamin with L-methylfolate may improve neurological symptom correction
Further metabolic evaluation may be required if biochemical correction remains incomplete.
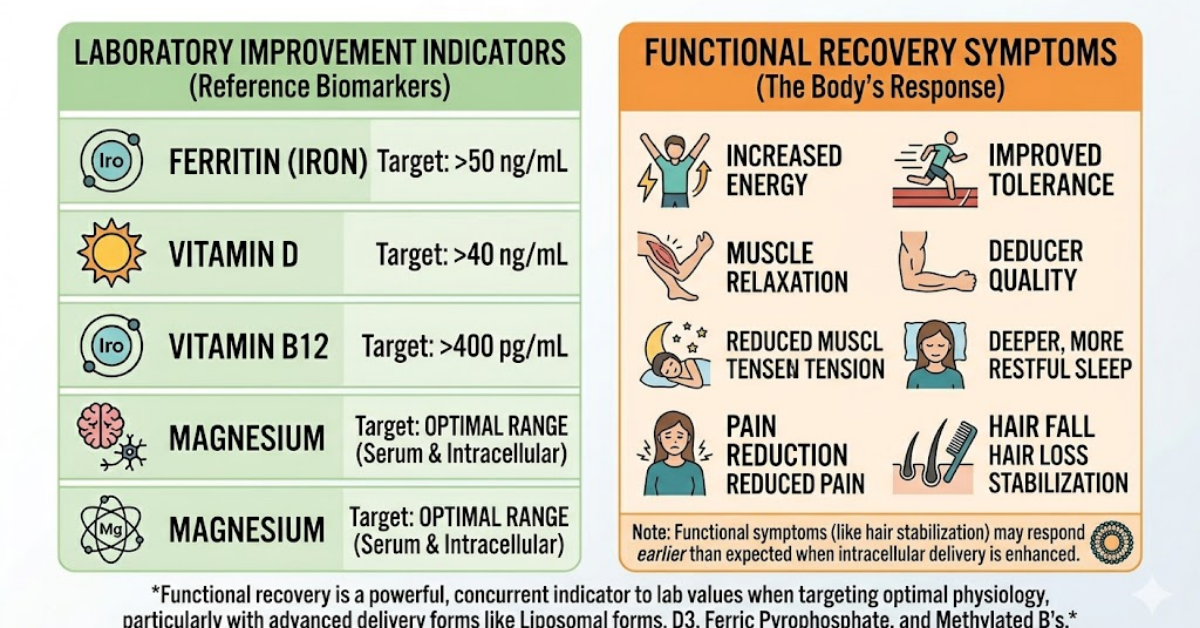
Objective Monitoring – Linking Lab Values with Symptoms
Successful correction should be evaluated using both laboratory improvement and functional recovery indicators such as:
- energy levels
- exercise tolerance
- muscle relaxation
- sleep quality
- pain reduction
- hair fall stabilization
Clinical experience suggests that when intracellular delivery improves—particularly with liposomal magnesium, vitamin D3, ferric pyrophosphate iron, or methylated B-vitamins—symptom improvement may occur earlier than expected based solely on serum biomarker normalization timelines.
Conventional vs Bioavailable Micronutrient Forms
Nutrient | Conventional Form | Bioactive Alternative | Clinical Advantage |
Iron | Ferrous sulfate | Liposomal ferric pyrophosphate (e.g., Precifer-type delivery) | Better tolerance, improved absorption |
Magnesium | Magnesium oxide | Liposomal magnesium (e.g., Mg+D3 combinations) | Improved intracellular uptake |
Vitamin D | Standard cholecalciferol tablets | Liposomal vitamin D3 (e.g., Mg+D3 structured support) | Enhanced bioavailability |
Vitamin B12 | Cyanocobalamin | Methylcobalamin | Improved neurological utilization |
Folate | Folic acid | L-methylfolate | Active metabolic participation |
Multivitamins | Conventional blends | Methylated complexes | Supports functional correction pathways |
Frequently Asked Questions
Yes. Vitamin B12, vitamin D, and magnesium deficiencies can reduce cellular energy production even when hemoglobin levels remain normal.
Yes. Urban lifestyle, indoor work patterns, and skin pigmentation reduce effective vitamin D synthesis despite adequate sunlight availability.
Yes. Ferritin below optimal levels affects hair follicle cycling even before anemia develops.
Most patients notice improvement in energy and nerve symptoms within 4–8 weeks of appropriate supplementation.
Yes. Magnesium supports neuromuscular relaxation and improves sleep quality in many individuals.
Maintenance doses may still be required depending on diet, lifestyle, and underlying metabolic risk factors.
Yes. Vitamin D plays a key role in immune signaling and inflammatory regulation even within borderline ranges.
Yes. Vitamin B12 is primarily obtained from animal-based foods.
Yes. Correction of vitamin D and magnesium often improves musculoskeletal discomfort.
Serum magnesium may not reflect intracellular levels accurately, so symptoms should also guide interpretation.
Yes. B12 and magnesium correction often improves concentration and mental clarity.
Yes, if ferritin is low and supplementation is medically appropriate.
Typically every 3 months during correction therapy.
Yes. Chronic stress increases magnesium utilization and affects nutrient metabolism.
Often yes, due to increased metabolic demand.
Yes. Gut inflammation significantly affects absorption of B12, magnesium, and iron.
They may improve bioavailability in individuals with compromised absorption.
Yes. Symptom improvement often precedes biochemical correction.
Depends on diet, lifestyle, and recurrence risk.
If severe fatigue, neurological symptoms, anemia, or unexplained weight loss occurs.