Obesity management is undergoing a rapid transformation with the increasing adoption of GLP-1 receptor agonists such as semaglutide and liraglutide. While these therapies have demonstrated significant effectiveness in reducing body weight and improving metabolic parameters, concerns regarding muscle loss, nutrient deficiency, affordability, long-term adherence, and rebound weight gain remain important—especially in the Indian population.
Emerging clinical practice patterns now suggest that GLP-1 microdosing combined with structured nutrition and targeted nutraceutical support may provide a safer, more sustainable strategy for long-term weight optimization.
This article reviews the scientific rationale behind GLP-1 microdosing, explains why adjunct bioactive nutraceuticals are increasingly important, and discusses how this combined strategy may improve outcomes in Indian patients.
Understanding GLP-1 Therapy in Weight Management
GLP-1 (Glucagon-Like Peptide-1) receptor agonists were originally developed for type 2 diabetes but are now widely used for obesity treatment.
Their mechanism includes:
- appetite suppression
• delayed gastric emptying
• improved insulin sensitivity
• reduced caloric intake
• enhanced satiety signaling
Clinical trials show weight reduction between 10% and 18% body weight in selected populations using full-dose GLP-1 protocols.
However, real-world use differs significantly from trial conditions.
Why the Concept of GLP-1 Microdosing Is Emerging
GLP-1 microdosing refers to the use of lower-than-standard therapeutic doses to achieve gradual metabolic improvements while minimizing adverse effects.
This approach is gaining interest because:
- gastrointestinal intolerance is reduced
- cost burden becomes manageable
- muscle loss risk may be lower
- adherence improves
- therapy becomes sustainable long-term
In India, where affordability and nutritional variability influence treatment success, microdosing strategies are particularly relevant.
Rather than aggressive appetite suppression, microdosing supports metabolic reprogramming with lifestyle integration.

Challenges with Standard GLP-1 Protocols in Indian Patients
Although effective, conventional GLP-1 dosing strategies may not always be ideal for Indian populations due to:
- lower baseline protein intake
- higher vegetarian prevalence
- frequent vitamin B12 deficiency
- variable micronutrient reserves
- limited access to structured diet supervision
These factors increase the risk of:
- fatigue
- muscle loss
- nutrient depletion
- treatment discontinuation
Therefore, adjunct nutritional strategies become essential.
Muscle Loss During GLP-1 Therapy: An Underestimated Concern
Recent body composition analyses indicate that 25–40% of weight loss during GLP-1 therapy may include lean body mass.
Loss of skeletal muscle has several consequences:
- reduced metabolic rate
- increased fatigue
- joint instability
- poor exercise tolerance
- higher risk of weight regain
This makes muscle-preserving interventions critical during pharmacologic weight reduction.
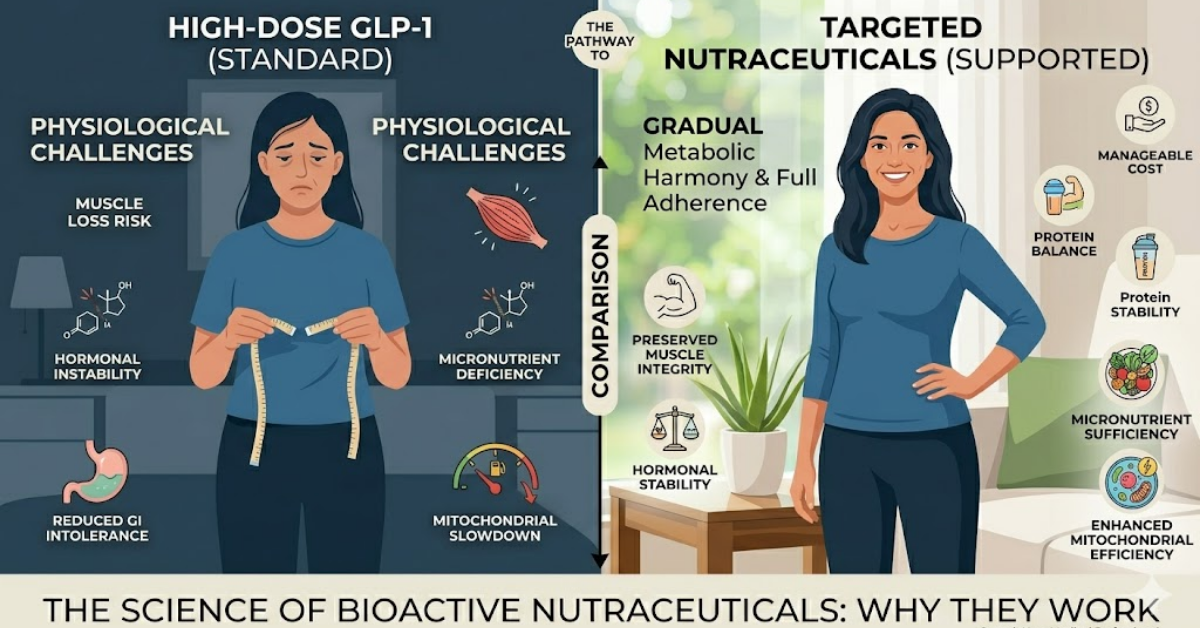
Why Bioactive Nutraceuticals Improve GLP-1 Outcomes
Targeted nutraceutical supplementation supports physiological adaptation during weight loss therapy.
These compounds help maintain:
- protein balance
- micronutrient sufficiency
- mitochondrial efficiency
- muscle integrity
- hormonal stability
When combined with GLP-1 microdosing, nutraceuticals act as metabolic stabilizers rather than weight-loss accelerators.
Role of Structured Meal Replacement Programs
One of the most effective adjunct strategies during GLP-1 therapy is structured meal replacement nutrition.
Protein-rich meal replacements help:
- preserve lean muscle mass
- maintain satiety
- prevent micronutrient deficiencies
- improve adherence to calorie control
In Indian vegetarian populations, this approach is particularly valuable.
Formulations combining:
- high-quality protein
- fiber
- micronutrients
- metabolic cofactors
may significantly improve treatment sustainability.
Essential Amino Acids and Muscle Preservation
Essential amino acid supplementation plays a central role in preventing sarcopenia during weight loss therapy.
Evidence suggests that adequate amino acid intake supports:
- muscle protein synthesis
- mitochondrial function
- exercise tolerance
- post-exercise recovery
Combining GLP-1 therapy with amino acid support helps shift weight loss toward fat mass rather than lean tissue loss.
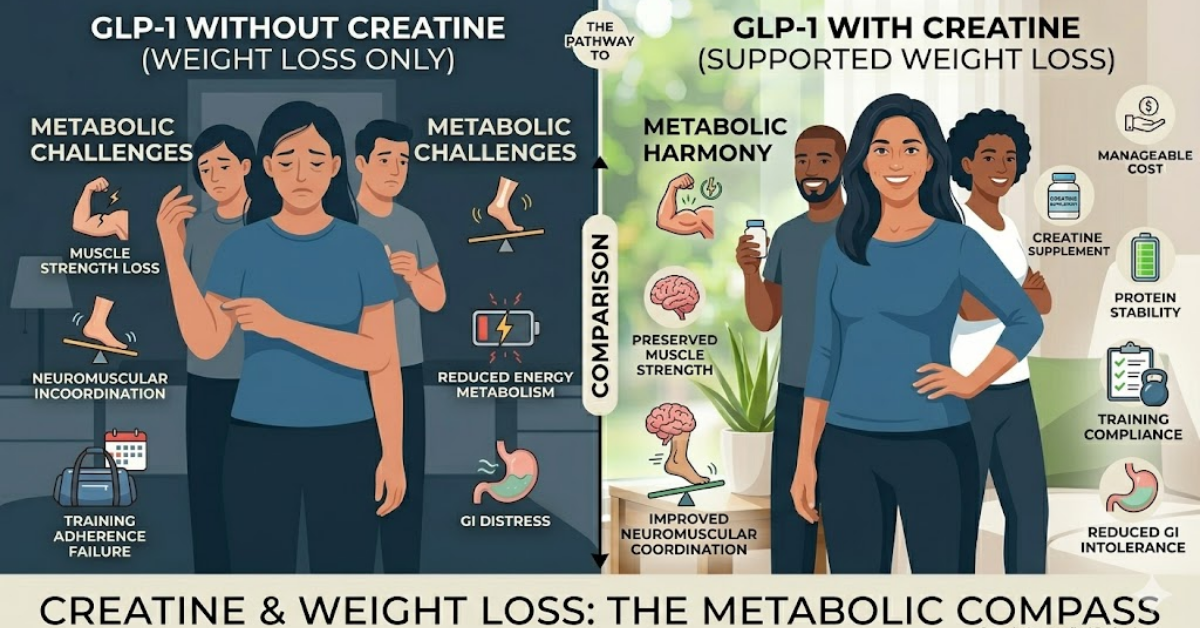
Creatine Supplementation and Metabolic Adaptation
Creatine is traditionally associated with sports performance but is increasingly recognized as beneficial during structured weight-loss programs.
Creatine supports:
- muscle strength preservation
- neuromuscular coordination
- energy metabolism
- training compliance
When included during GLP-1-assisted weight reduction, creatine may help maintain functional performance capacity.
Micronutrient Support During GLP-1 Therapy
Reduced appetite during GLP-1 treatment often leads to unintended micronutrient insufficiency.
Common deficiencies include:
- vitamin B12
- vitamin D
- iron
- magnesium
Correction of these deficiencies improves:
energy levels
neuromuscular stability
metabolic efficiency
training tolerance
This is especially relevant in Indian vegetarian populations.
Liposomal Nutraceutical Technologies and Absorption Advantages
Advanced delivery systems such as liposomal formulations improve bioavailability of key micronutrients.
Liposomal delivery enhances:
- intestinal absorption
- cellular uptake
- tolerance in sensitive individuals
These technologies are particularly useful during calorie-restricted phases of weight reduction.
GLP-1 Microdosing in Patients with Osteoarthritis and Joint Pain
Many individuals seeking weight reduction therapy also suffer from knee pain or spine-related conditions.
Rapid weight loss without muscle preservation may worsen joint instability.
Combining GLP-1 microdosing with:
- physiotherapy
- muscle strengthening
- collagen-supportive nutrition
helps improve both metabolic and orthopedic outcomes simultaneously.
Role of Physiotherapy During Pharmacologic Weight Reduction
Structured movement therapy is essential during weight loss interventions.
Physiotherapy supports:
- muscle retention
- joint protection
- balance improvement
- injury prevention
This integrated strategy improves long-term sustainability compared with medication alone.
Preventing Weight Regain After GLP-1 Therapy
One of the most important limitations of GLP-1 therapy is rebound weight gain after discontinuation.
This occurs because:
- appetite returns
- metabolic rate declines
- muscle mass decreases
Microdosing combined with nutraceutical support helps transition patients toward lifestyle-based maintenance strategies.

Who Benefits Most from GLP-1 Microdosing Strategies
Microdosing approaches may be particularly suitable for:
- patients with BMI 27–35
- early metabolic syndrome
- polycystic ovarian syndrome
- prediabetes
- central obesity with joint pain
These individuals often benefit from gradual metabolic correction rather than aggressive pharmacologic appetite suppression.
Indian Dietary Patterns and Their Influence on GLP-1 Outcomes
Indian dietary habits influence treatment response significantly.
Low protein intake is common in vegetarian populations and may increase muscle loss risk during weight reduction.
Integrating:
- protein supplementation
- amino acid support
- micronutrient correction
improves metabolic adaptation.
Emerging Evidence Supporting Integrated Metabolic Strategies
Recent clinical observations suggest that combining pharmacologic therapy with targeted nutritional support produces:
- better adherence
- lower side-effect rates
- improved body composition
- greater sustainability
Although large-scale randomized trials are still evolving, early real-world outcomes support this integrated approach.
Safety Considerations with GLP-1 Therapy
Common side effects include:
- nausea
- constipation
- early satiety
Less frequent concerns include:
- gallbladder disease
- muscle loss
- bone density changes
Microdosing strategies may reduce the incidence of these complications.
The Future of Precision Obesity Management in India
Obesity care is shifting toward personalized metabolic correction strategies.
Future models will likely combine:
- low-dose pharmacotherapy
- nutraceutical optimization
- gut microbiome modulation
- structured physiotherapy
- protein-preserving nutrition
This integrative approach offers a safer pathway toward sustainable weight reduction.
Conclusion
GLP-1 receptor agonists represent one of the most significant advances in obesity management in recent decades. However, long-term success depends not only on pharmacologic appetite suppression but also on preservation of muscle mass, correction of micronutrient deficiencies, and structured lifestyle integration.
GLP-1 microdosing combined with targeted bioactive nutraceutical support offers a promising strategy for improving treatment tolerance, reducing complications, and enhancing sustainability—particularly in the Indian population.
As metabolic medicine evolves, personalized nutrition and rehabilitation-based interventions will play an increasingly important role in optimizing outcomes for patients undergoing weight-loss therapy.
Frequently Asked Questions
GLP-1 microdosing refers to the use of lower-than-conventional doses of GLP-1 receptor agonists to gradually improve appetite regulation, insulin sensitivity, and metabolic function without inducing excessive appetite suppression or gastrointestinal side effects. Unlike full-dose protocols used in obesity pharmacotherapy trials, microdosing supports slower, steadier fat loss and improves treatment adherence. In Indian clinical practice, this approach is increasingly combined with structured nutrition and protein support strategies for better sustainability.
Yes, when combined with dietary correction and muscle-preserving strategies, GLP-1 microdosing can produce meaningful and sustainable fat loss. Rather than rapid appetite shutdown, it supports metabolic reset and behavioral adaptation. Outcomes improve further when combined with structured meal replacement programs such as MAXLITE, which help maintain satiety and micronutrient intake during calorie restriction.
Rapid weight loss often leads to loss of lean muscle mass along with fat mass. Studies suggest that up to 25–40% of weight reduction during GLP-1 therapy may involve muscle loss if protein intake is inadequate. Muscle preservation is critical because skeletal muscle determines resting metabolic rate. Supplementation with essential amino acids such as EAA MAX supports muscle protein synthesis and helps shift weight loss toward fat rather than lean tissue.
Yes. Nutraceuticals support metabolic adaptation, reduce fatigue, preserve muscle mass, and improve treatment tolerance. Structured supplementation ensures that reduced appetite does not lead to nutrient deficiency. Programs incorporating protein support (MAXLITE), amino acids (EAA MAX), creatine support, and gut microbiome optimization (PRIZIBIOM) can significantly improve sustainability of weight reduction.
GLP-1 therapies reduce appetite, which often unintentionally lowers protein intake. Low protein intake increases the risk of muscle loss and fatigue. Structured protein supplementation using balanced meal replacements like MAXLITE helps maintain lean mass, improve satiety, and stabilize energy levels during weight-loss phases.
- What role do essential amino acids play in GLP-1-assisted weight loss?
Yes. Creatine is increasingly recognized as a metabolic support supplement during structured weight loss programs. Creatine Effervescent Granules help maintain muscle strength, improve neuromuscular efficiency, and support exercise adherence. This is particularly useful for individuals beginning physiotherapy or strength training alongside GLP-1 microdosing
Fatigue may result from reduced calorie intake, inadequate protein consumption, micronutrient deficiencies, or muscle loss. Supporting nutritional intake with structured meal replacement programs and amino acid supplementation helps reduce this fatigue and improves functional energy levels.
GLP-1 receptors interact closely with the gut–brain axis. A healthy gut microbiome improves metabolic signaling and treatment response. Probiotic supplementation such as PRIZIBIOM, which contains clinically validated strains, helps improve digestion, reduce bloating, enhance nutrient absorption, and support metabolic balance during weight loss.
Yes, but it should be combined with muscle-preserving strategies. Rapid weight loss without strength training may worsen joint instability. Integrating physiotherapy with nutraceutical support such as amino acids and creatine improves joint stability and functional recovery during weight reduction.
Weight regain occurs when appetite returns and metabolic rate declines due to muscle loss. Structured transition plans that include protein supplementation, microbiome support, and strength training help maintain long-term metabolic stability after discontinuation.
Yes. Balanced meal replacements such as MAXLITE provide controlled calories along with essential nutrients, fiber, and protein. This prevents nutrient deficiencies and stabilizes appetite signals, reducing dizziness, weakness, and fatigue during treatment.
GLP-1 microdosing can be particularly useful in individuals with insulin resistance or prediabetes. When combined with targeted nutrition and probiotic support such as PRIZIBIOM, it helps improve glucose regulation and metabolic flexibility.
Creatine supports cellular energy metabolism and muscle contraction efficiency. Supplementation with Creatine Effervescent Granules improves exercise tolerance, allowing patients to maintain activity levels during weight loss programs.
Yes. Reduced appetite may unintentionally decrease intake of vitamin B12, iron, magnesium, and protein. Structured supplementation and meal replacement programs help prevent these deficiencies and improve treatment tolerance.
Yes, but vegetarian patients require careful monitoring of protein and vitamin B12 intake. Supplementation with amino acids such as EAA MAX and structured protein support using MAXLITE improves outcomes significantly in vegetarian populations.
Probiotics improve gut barrier function, reduce inflammation, and enhance nutrient absorption. PRIZIBIOM supports microbiome balance, which helps regulate appetite signaling and improves response to metabolic therapies.
Individuals with moderate obesity, early metabolic syndrome, PCOS, or weight-related joint pain often benefit from gradual metabolic correction rather than aggressive appetite suppression. Microdosing combined with nutraceutical support improves adherence and reduces adverse effects.
Yes. Combining GLP-1 microdosing with physiotherapy improves muscle preservation, mobility, and joint stability. Nutritional support with amino acids and creatine further enhances rehabilitation outcomes.
The future of obesity care lies in precision metabolic medicine. Rather than relying solely on pharmacotherapy, integrated strategies combining GLP-1 microdosing, structured nutrition, microbiome support, and muscle-preserving supplementation such as MAXLITE, EAA MAX, Creatine Effervescent Granules, and PRIZIBIOM are expected to produce safer and more sustainable long-term results.