Gut health has become one of the most discussed topics in modern medicine and nutrition. Over the past decade, scientific research has revealed that the digestive tract is not simply responsible for digestion—it also influences immunity, metabolism, brain function, and inflammation.
The human gut contains trillions of microorganisms collectively known as the gut microbiome. These microbes play a vital role in nutrient absorption, immune defense, and protection against harmful pathogens. When this delicate microbial ecosystem becomes imbalanced, a condition known as gut dysbiosis can occur.
Dysbiosis has been linked to numerous digestive and metabolic disorders including:
- Digestive complaints
- Irritable Bowel Syndrome (IBS)
- Small Intestinal Bacterial Overgrowth (SIBO)
- Inflammatory bowel conditions
- Food intolerance
- Chronic fatigue and brain fog
Fortunately, emerging evidence suggests that many gut disorders can be improved through personalized dietary interventions, targeted nutritional supplements, and lifestyle modifications.
This article explores practical strategies for restoring gut balance and highlights five real-world case examples demonstrating how simple interventions can significantly improve gut health.

What Is Gut Dysbiosis?
Gut dysbiosis refers to an imbalance between beneficial and harmful microorganisms in the digestive tract. In a healthy gut microbiome, beneficial bacteria help digest food, produce vitamins, regulate immune function, and protect against pathogens.
However, several factors can disrupt this balance:
- Antibiotic use
- Highly processed diets
- Low fiber intake
- Chronic stress
- Sleep deprivation
- Excess sugar consumption
- Environmental toxins
When dysbiosis occurs, harmful microbes may proliferate while beneficial bacteria decline. This imbalance can contribute to symptoms such as:
- Bloating after meals
- Excess gas
- Food intolerance
- Loose stools or constipation
- Acid reflux
- Fatigue and brain fog
Research indicates that alterations in gut microbiota composition play a central role in IBS pathophysiology.
Reference: Simrén M et al., Gut microbiota in IBS, Gastroenterology Clinics of North America.
The Gut-Brain-Immune Axis
Modern research has demonstrated that the gut is deeply connected with the brain and immune system.
Approximately 70–80% of immune cells reside in the gastrointestinal tract. The gut microbiome helps regulate immune responses and inflammation throughout the body.
The gut-brain axis refers to the communication network linking the digestive tract and the central nervous system. Changes in microbiome composition may influence mood, stress response, and cognitive function.
Reference: Cryan JF et al., The Microbiota-Gut-Brain Axis, Nature Reviews Neuroscience.
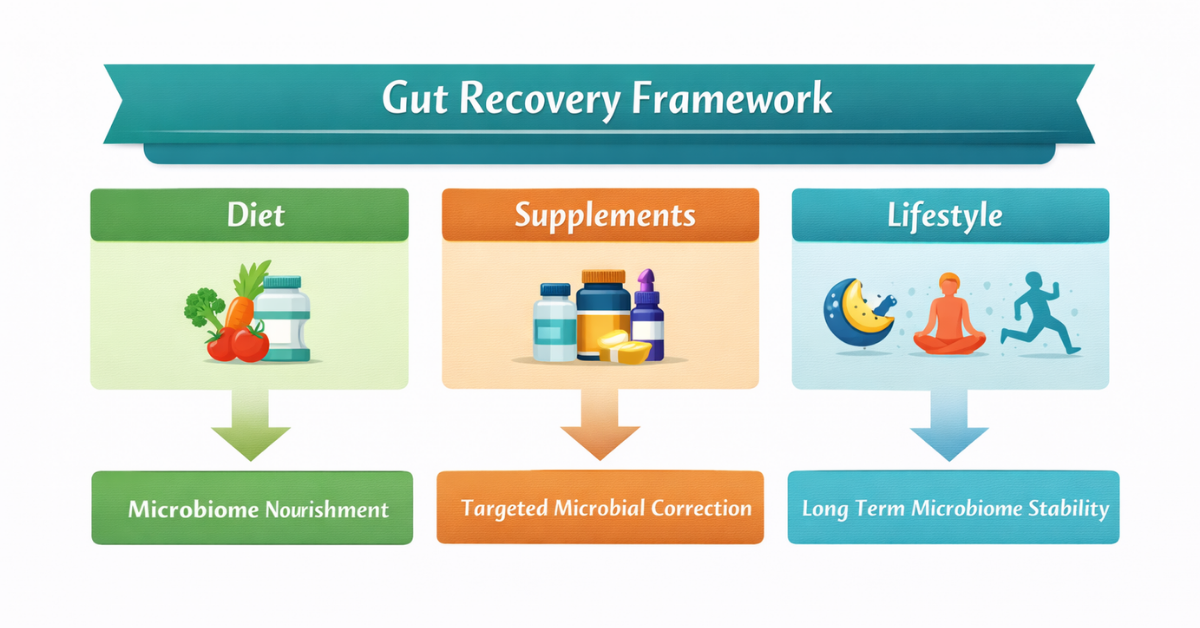
The Three Pillars of Gut Recovery
Restoring gut health typically requires addressing multiple factors simultaneously. Three key pillars play an essential role in microbiome recovery:
- Personalized diet
- Targeted nutraceuticals
- Lifestyle modifications
When implemented together, these strategies can significantly improve digestive symptoms and restore microbial balance.
Pillar 1: Personalized Diet Plans for Gut Health
Diet is the most powerful factor influencing the gut microbiome.
Different dietary patterns can either promote microbial diversity or encourage dysbiosis. Personalized nutrition plans can therefore play a crucial role in managing digestive disorders.
Low-FODMAP Diet for IBS
The Low-FODMAP diet is widely used to manage symptoms of IBS. FODMAPs are fermentable carbohydrates that can cause gas production and bloating in sensitive individuals.
Clinical studies have shown that a low-FODMAP diet can improve IBS symptoms in approximately 70% of patients.
Reference: Halmos EP et al., Low FODMAP diet reduces IBS symptoms, Gastroenterology.
Mediterranean Diet and Gut Microbiome
The Mediterranean diet, rich in vegetables, olive oil, whole grains, and legumes, has been shown to increase microbial diversity and reduce inflammation.
This dietary pattern encourages the growth of beneficial bacteria that produce short-chain fatty acids, which protect the intestinal lining.
Fiber and Prebiotic Foods
Dietary fiber acts as a prebiotic, nourishing beneficial gut bacteria. Foods that support microbiome health include:
- Vegetables
- Whole grains
- Legumes
- Garlic and onions
- Bananas
- Fermented foods such as yogurt and kefir
Pillar 2: Targeted Nutraceutical Support
While diet provides the foundation for gut health, targeted nutraceuticals can accelerate recovery by supporting specific physiological mechanisms.
Below are examples of nutritional interventions that can support microbiome balance.
PRIZIBIOM – Microbiome Restoration
PRIZIBIOM provides 10 high-potency freeze-dried probiotic strains designed to support microbiome diversity and digestive health.
Potential benefits include:
- Restoring beneficial gut bacteria
- Reducing bloating and gas
- Supporting immune function
- Enhancing nutrient absorption
Clinical evidence suggests probiotics may improve symptoms of IBS and other functional gastrointestinal disorders.
Reference: Ford AC et al., Probiotics in IBS, American Journal of Gastroenterology.
PRIZIBIOM Lite – Digestive Support with Probiotics and Enzymes
PRIZIBIOM Lite combines probiotics with digestive enzymes, glutamine, and liposomal zinc.
This formulation supports:
- Efficient food digestion
- Gut barrier repair
- Improved nutrient absorption
- Reduced post-meal heaviness
Glutamine is particularly important for maintaining the health of intestinal epithelial cells.
SIBOWEL – Microbial Balance Support
SIBOWEL contains a combination of plant-derived compounds known for their antimicrobial and digestive properties.
Key ingredients include:
- Berberine
- Oregano extract
- Ginger extract
- Caprylic acid
These compounds may help regulate microbial overgrowth and reduce fermentation in the small intestine.
Reference: Chedid V et al., Herbal therapy for SIBO, Global Advances in Health and Medicine.
LF-MAX – Liposomal Lactoferrin
Lactoferrin is a multifunctional protein with antimicrobial and anti-inflammatory properties.
Research suggests lactoferrin may inhibit the growth of H. pylori, a bacterium associated with gastritis and ulcers.
Reference: Di Mario F et al., Lactoferrin and H. pylori, Digestive and Liver Disease.
The liposomal delivery system helps improve stability and bioavailability.
Pillar 3: Lifestyle Factors That Influence Gut Health
Lifestyle habits strongly influence microbiome composition.
Sleep Quality
Poor sleep patterns can disrupt circadian rhythms and negatively affect gut bacteria.
Stress Management
Chronic stress affects the gut-brain axis and can alter microbial balance.
Techniques such as meditation, breathing exercises, and yoga may help regulate stress responses.
Physical Activity
Regular exercise has been associated with increased microbial diversity and improved digestive function.
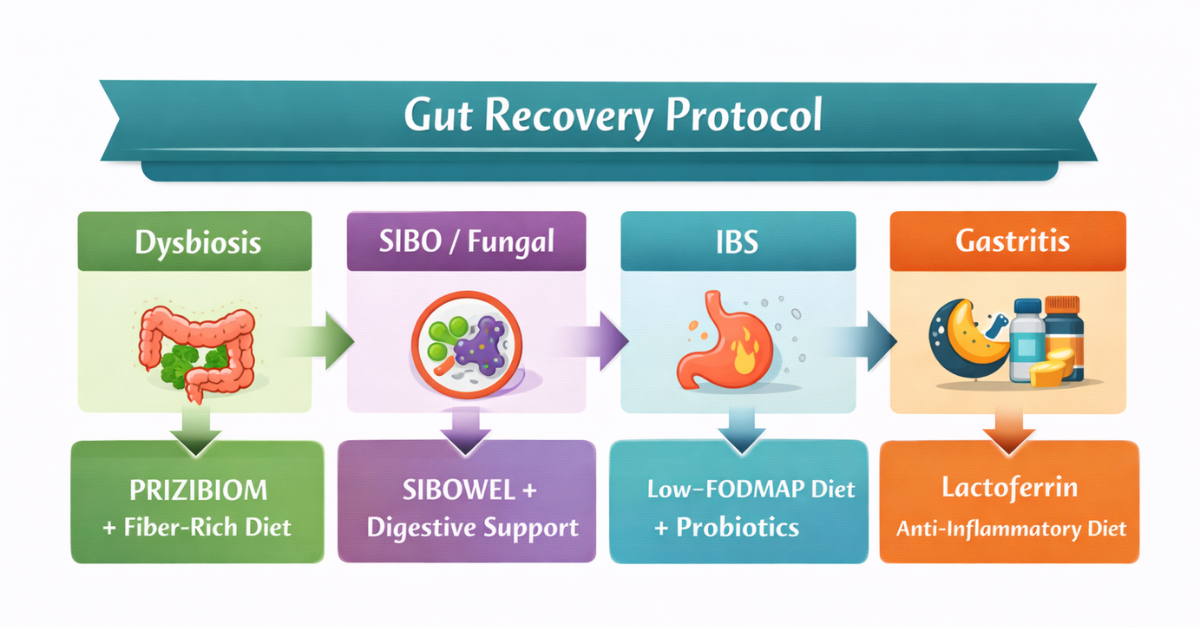
Five Case Studies: Simple Approaches That Delivered Results
The following cases were documented by Mary Ebhraham, Kochi, and reviewed by Dr. Sarath Chandra, Functional Medicine Specialist, Bangalore.
Case Study 1: Post-Antibiotic Dysbiosis
Patient: Female, 32
Symptoms
Bloating
Irregular bowel movements
Fatigue
Intervention
High-fiber diet
Fermented foods
PRIZIBIOM
PRIZIBIOM Lite
Outcome
After six weeks, bowel movements normalized and bloating significantly improved.
Case Study 2: IBS-Diarrhea Type
Patient: Male, 41
Symptoms
Loose stools
Gas
Food sensitivity
Intervention
Low-FODMAP diet
PRIZIBIOM
CUCIMAX (curcumin support)
Outcome
Symptoms improved within four weeks.
Case Study 3: SIBO-Like Symptoms
Patient: Female, 38
Symptoms
Severe bloating
Gas after meals
Brain fog
Intervention
SIBOWEL
PRIZIBIOM Lite
Reduced sugar intake
Outcome
Significant improvement in bloating within eight weeks.
Case Study 4: H. pylori-Related Gastritis
Patient: Male, 45
Symptoms
Burning sensation
Nausea
Acidity
Intervention
LF-MAX
CUCIMAX
Anti-inflammatory diet
Outcome
Gastric discomfort improved within six weeks.
Case Study 5: IBS-Constipation
Patient: Female, 36
Symptoms
Constipation
Bloating
Fatigue
Intervention
High-fiber diet
Hydration
PRIZIBIOM Lite
Outcome
Regular bowel movements restored after five weeks.
Key Takeaway
Gut health is influenced by diet, lifestyle, and microbial balance. Many digestive disorders—including IBS, dysbiosis, and post-antibiotic gut disturbances—can improve significantly through personalized strategies.
Combining targeted nutraceuticals, dietary changes, and healthy lifestyle practices offers a practical and effective approach to restoring digestive wellness.
As emphasized by Dr. Sarath Chandra, functional medicine approaches that address root causes—rather than merely treating symptoms—can produce sustainable improvements in gut health.
Frequently Asked Questions
1 What is gut dysbiosis
Bloating, gas, constipation, diarrhea, fatigue.
Diet plays a major role but may need to be combined with targeted supplements.
Fiber-rich foods, fermented foods, vegetables.
Certain high-FODMAP foods.
A diet that reduces fermentable carbohydrates.
Certain strains can help regulate gut bacteria.
Excess bacterial growth in the small intestine.
Studies suggest antimicrobial effects.
Yes, through the gut-brain axis.
They may improve food breakdown and reduce heaviness.
Typically 4–8 weeks depending on severity.
Most nutraceuticals are safe when used appropriately.
Yes, most immune cells reside in the gut.
Yes, they can reduce beneficial bacteria.
Yes, it increases microbial diversity.
Yes, they provide natural probiotics.
Research suggests anti-inflammatory benefits.
Symptoms can often be managed effectively.
Yes, medical consultation is recommended.





