Iron supplementation is a cornerstone of antenatal care worldwide. Yet in routine clinical practice, many pregnant women continue to have low hemoglobin levels despite taking iron tablets regularly. This creates uncertainty for patients and an important diagnostic challenge for clinicians.
An important clinical reality is often overlooked:
Not all anemia during pregnancy responds to standard iron therapy.
Understanding why hemoglobin sometimes fails to improve requires looking beyond dosage and compliance toward physiology, inflammation, micronutrient status, and differences in iron absorption mechanisms.

Why does anemia persist in pregnancy despite iron supplements?
Anemia may persist during pregnancy despite iron supplementation because not all pregnancy anemia is caused by iron deficiency alone. Common reasons include inflammation-related iron blockade (hepcidin effect), vitamin B12 or folate deficiency, late diagnosis in the third trimester, reduced absorption due to interactions with calcium or thyroid medications, and functional iron deficiency, in which iron stores are present but unavailable for hemoglobin production.
The Burden of Anemia in Pregnancy Remains High Despite Supplementation
According to NFHS-5, approximately 52.2% of pregnant women in India are anaemic, making it one of the most persistent maternal health concerns nationally.
Globally, pregnancy anemia affects roughly 40–60% of women, even in regions where supplementation programs are widely implemented.
This suggests that routine iron therapy alone does not address all causes of pregnancy-related anemia.
Evidence-Based Indian Burden Data
Indicator | Value | Source |
Pregnant women with anemia (India) | 52.2% | NFHS-5 national survey |
Global pregnancy anemia prevalence | 40–60% | multicountry estimates cited in obstetric RCT background |
Expected Hemoglobin Rise With Standard Oral Iron Therapy
In uncomplicated iron deficiency anemia:
oral iron typically increases hemoglobin by about 1–2 g/dL over 4–8 weeks
Randomized antenatal studies show:
~0.2–0.6 g/dL rise within 2 weeks
~1.3 g/dL rise by 4 weeks
~1.5–2 g/dL rise by 6–8 weeks
However, clinical trials also demonstrate that only about half to three-quarters of patients achieve target hemoglobin levels with oral therapy alone.
This variability explains why reassessment during treatment is essential.
Evidence-Based Clinical Review Table
Hemoglobin Response With Oral Iron in Pregnancy
Parameter | Evidence-Based Range | Source Evidence |
Hb rise at 2 weeks | ~0.2–0.6 g/dL | IV vs oral comparison trial showed 0.23 g/dL rise oral group at 14 days |
Hb rise at 4 weeks | ~1.0–1.5 g/dL | Oral therapy arm showed 1.3 g/dL rise by day 28 |
Hb rise at 6 weeks | ~1.5–2.0 g/dL | Ferrous sulfate arm showed 1.7 g/dL rise at 6 weeks |
Target Hb achievement rate | ~54–72% | 54% reached Hb ≥11 g/dL with oral therapy vs 76% IV group |
GI side-effect frequency | up to ~36% | Reported gastrointestinal effects in oral therapy cohort |
Non-compliance rates | ~10% | Observed in oral iron arm of RCT |
Interpretation
These data explain why a clinically meaningful subgroup of pregnancies fails to normalize hemoglobin with tablets alone.
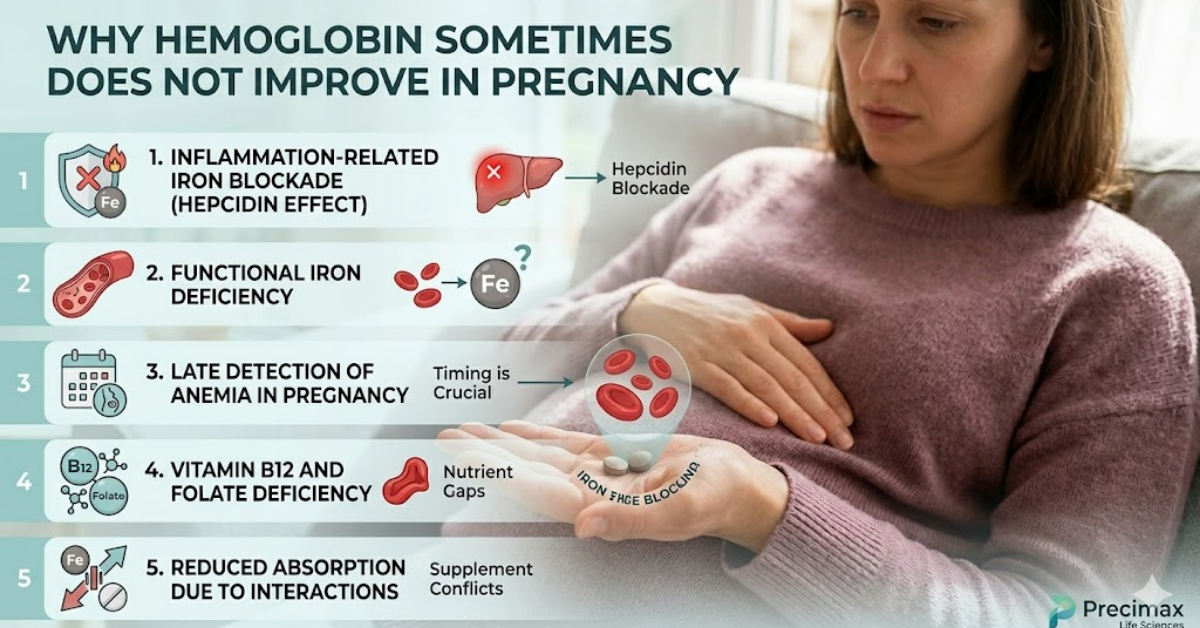
When Hemoglobin Does Not Improve Despite Iron Tablets
Persistent anemia during supplementation usually reflects one or more underlying mechanisms rather than treatment failure alone.
- Inflammation-Related Iron Blockade (Hepcidin Effect)
Iron absorption is regulated by hepcidin, a hormone that increases during inflammatory states and prevents iron entry into circulation.
This mechanism is common in pregnancies complicated by:
- gestational diabetes
- hypertensive disorders
- maternal obesity
- subclinical infection
In such cases, iron may be present but unavailable for hemoglobin production.
- Functional Iron Deficiency
Functional iron deficiency occurs when iron stores appear adequate but cannot be mobilized effectively.
Typical pattern:
- normal ferritin
- low hemoglobin
- reduced transferrin saturation
This is frequently mistaken for poor compliance with supplementation.
- Late Detection of Anemia in Pregnancy
Iron demand increases sharply in the third trimester. When anemia is detected late, there may not be sufficient time for oral therapy alone to restore hemoglobin before delivery.
Early antenatal screening significantly improves correction rates.
- Vitamin B12 and Folate Deficiency
Iron is only one component of red blood cell production.
- Deficiency of:
- vitamin B12
- folate
can prevent hemoglobin improvement even when iron intake is adequate.
This is particularly relevant in vegetarian populations.
- Reduced Absorption Due to Supplement Interactions
- Conventional iron salts compete with several dietary components for absorption.
- Common inhibitors include:
- calcium supplements
- milk
- tea and coffee
- thyroid medication
- Spacing these appropriately improves treatment response.
Importantly, newer formulations such as liposomal iron use alternative uptake pathways and are theoretically less affected by mineral competition compared with traditional ferrous salts.
How long should iron tablets take to increase hemoglobin during pregnancy?
In uncomplicated iron deficiency anemia, hemoglobin typically increases by about 1–2 g/dL within 4–8 weeks of starting oral iron therapy. If hemoglobin does not rise by at least 1 g/dL after 3 weeks, further evaluation for inflammation, vitamin deficiencies, or absorption issues is recommended.
Gastrointestinal Intolerance Limits Effectiveness of Standard Iron Therapy
Ferrous salts remain the most widely prescribed therapy but are frequently associated with:
- constipation
- nausea
- gastric irritation
- metallic taste
Clinical studies report gastrointestinal side effects in up to one-third of pregnant patients, contributing to incomplete adherence.
Even mild intolerance can reduce treatment effectiveness.
When Injectable Iron Therapy Is Considered
Intravenous iron is typically recommended when faster correction is required or oral therapy is ineffective.
Common indications include:
- hemoglobin below 9 g/dL after mid-pregnancy
- Poor response after 3–4 weeks of oral therapy
- intolerance to oral iron
- late detection of anemia
- malabsorption syndromes
Injectable therapy generally produces faster hemoglobin correction than oral supplementation.
Hemoglobin Response With Injectable Iron in Pregnancy
Injectable Iron | Hb Rise | Correction Rate | Supporting Study |
Iron sucrose | 1.9 g/dL in 4 weeks | 76% achieved Hb ≥11 g/dL | RCT comparison with oral therapy |
Ferric carboxymaltose | 2.6 g/dL in 6 weeks | Higher correction vs oral iron | Indian RCT (362 patients) |
Ferric carboxymaltose (real-world India cohort) | 2.74–3.6 g/dL in 4 weeks | Strong response across severities | Multicenter PROMISE study (n=1191) |
Ferric carboxymaltose vs iron sucrose | +0.89 g/dL additional Hb improvement | Superior ferritin correction | Meta-analysis of RCTs |
Interpretation
Injectable iron typically produces:
- faster Hb rise
- higher ferritin restoration
- better third-trimester correction success
but still does not guarantee universal response.
Evidence-Based Comparison
Oral vs Injectable Iron Success Rates
Outcome | Oral Iron | Injectable Iron | Evidence |
Hb ≥11 g/dL achievement | ~54% | ~76% | Comparative RCT |
Hb rise (4–6 weeks) | ~1.3–1.7 g/dL | ~2.6–3.0 g/dL | Multiple RCT datasets |
GI side effects | up to 36% | minimal | RCT comparison |
Rapid correction suitability | Limited | High | Clinical comparative trials |
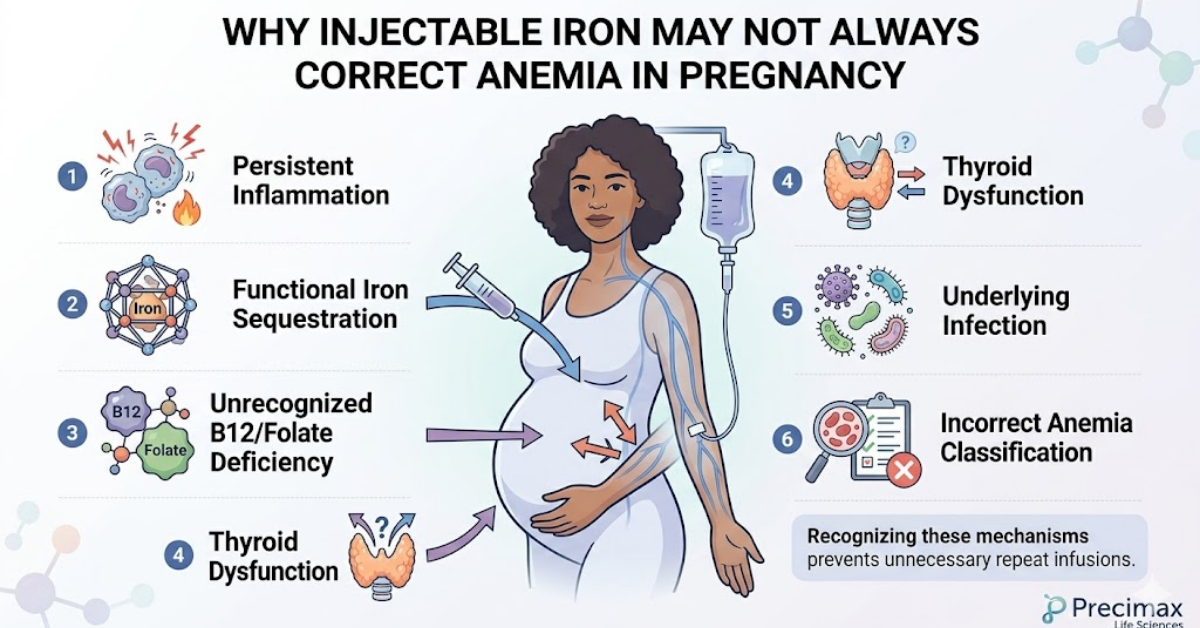
Why Injectable Iron Does Not Always Solve the Problem
Even intravenous therapy may produce incomplete correction in some pregnancies.
Possible reasons include:
- persistent inflammation
- functional iron sequestration
- unrecognized B12 deficiency
- thyroid dysfunction
- infection
- incorrect anemia classification
Recognizing these mechanisms prevents unnecessary repeat infusions.
When are iron injections needed during pregnancy?
Iron injections are usually recommended when hemoglobin falls below 9 g/dL after mid-pregnancy, when oral iron is not tolerated, when response to tablets is inadequate after 3–4 weeks, or when anemia is detected late and rapid correction is required before delivery.
Evidence-Based Dropout / Intolerance Estimates
Therapy | Dropout / Adverse Effect Pattern | Evidence |
Oral ferrous salts | GI side effects ~36% | RCT pregnancy cohort |
Oral therapy non-compliance | ~10% | Same RCT dataset |
Ferric carboxymaltose IV | ~8.6% mild adverse effects | Multicenter observational study (India) |
Serious adverse reactions IV iron | rare | Meta-analysis safety review |
Why Ferritin Alone May Not Reflect Iron Availability
Ferritin reflects stored iron but not necessarily usable iron.
During inflammation:
- ferritin may remain normal or elevated
- iron delivery to bone marrow remains impaired
This explains why hemoglobin sometimes fails to improve despite apparently adequate stores.
Special Clinical Situations Where Standard Iron Therapy Often Underperforms
Certain pregnancy contexts are associated with reduced response to supplementation:
- gestational diabetes
- hypertensive pregnancy disorders
- maternal obesity
- short interpregnancy interval
- vegetarian low-ferritin baseline
- thyroid disorders
- recurrent anemia across pregnancies
Recognizing these situations early supports individualized treatment planning.
Emerging Oral Iron Approaches That Improve Tolerability and Absorption
Newer oral iron delivery systems are designed to address limitations of conventional ferrous salts.
These include:
- liposomal iron
- ferric pyrophosphate
- lactoferrin-assisted iron delivery
Such formulations may be useful in women who experience intolerance with standard preparations or require longer-term supplementation support.
Because liposomal iron is absorbed via phospholipid vesicle transport rather than classical ionic pathways, its interaction with calcium and competing minerals is believed to be lower than that seen with conventional iron salts.
Why Monitoring Treatment Response Is Essential During Pregnancy
A structured follow-up strategy improves outcomes.
Typical approach:
- start oral therapy
- reassess hemoglobin after 3 weeks
- evaluate ferritin if response inadequate
- check B12 when indicated
- consider alternative formulations if intolerance occurs
- consider injectable therapy when correction is urgent
This stepwise evaluation prevents delayed correction before delivery.
Why Iron Therapy Should Continue After Hemoglobin Normalizes
Normalization of hemoglobin does not guarantee restoration of iron stores.
Continuation of supplementation for 6–8 weeks after correction helps:
- restore maternal reserves
- support fetal iron transfer
- reduce postpartum anemia risk
Moving Toward Individualized Management of Pregnancy Anemia
Evidence increasingly shows that pregnancy anemia is not always caused by iron deficiency alone.
Treatment success depends on identifying:
- timing of diagnosis
- inflammation status
- store availability
- deficiencies
- absorption limitations
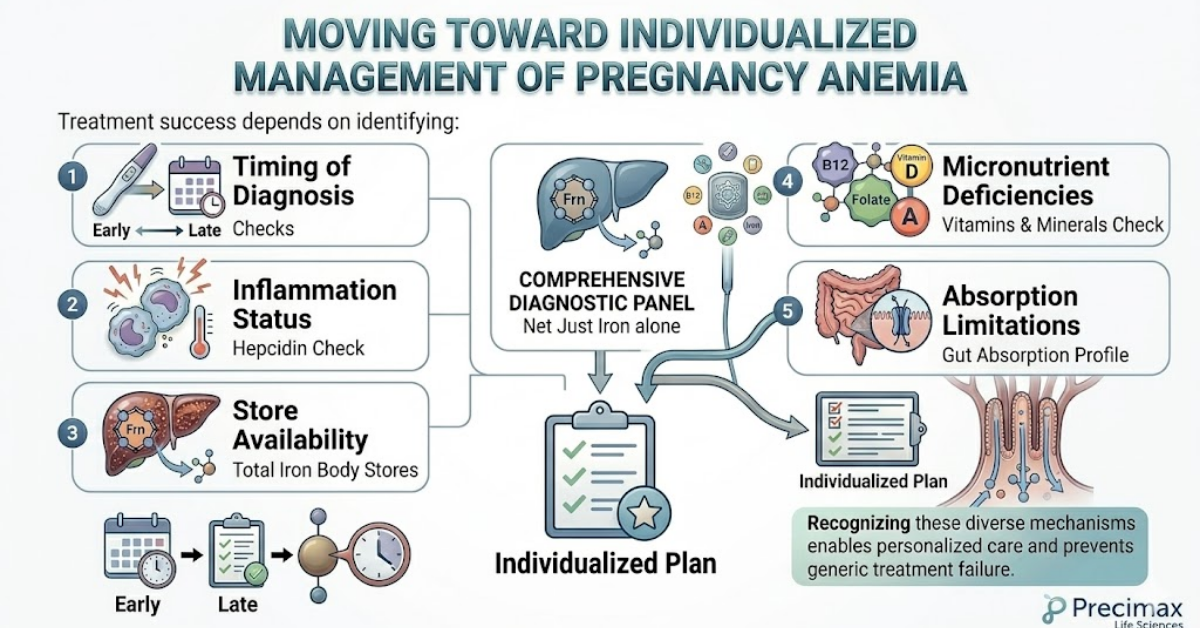
Recognizing why standard iron therapy sometimes fails allows earlier correction and better maternal and fetal outcomes.
Frequently Asked Questions
This may occur due to inflammation, vitamin B12 deficiency, thyroid disorders, calcium interaction, poor absorption, or functional iron deficiency where stored iron cannot be used effectively.
Hemoglobin typically rises by 1–2 g/dL within 4–8 weeks. A rise of at least 1 g/dL after 3 weeks suggests good response.
Yes. Pregnancy anemia can also result from B12 deficiency, folate deficiency, inflammation, infections, thyroid disease, or chronic nutritional insufficiency.
If hemoglobin does not improve after 3 weeks of treatment, additional tests such as ferritin, vitamin B12, and inflammation markers may be required.
Yes, calcium can reduce absorption of conventional iron salts. Spacing doses improves effectiveness.
Liposomal iron uses a different absorption pathway and is theoretically less affected by mineral competition compared with conventional ferrous salts.
Iron injections are considered when hemoglobin is below 9 g/dL, oral therapy is not tolerated, or rapid correction is needed late in pregnancy.
Yes. Inflammation associated with gestational diabetes can reduce iron availability for hemoglobin production.
This condition is called functional iron deficiency, where stored iron cannot be effectively used by the body.
Yes. Continuing supplementation for 6–8 weeks helps restore iron stores and prevent recurrence.