For decades, the standard response to a diagnosis of osteopenia or osteoporosis has been simple: “Take more calcium.” However, recent clinical researched in cardiovascular research are forcing a radical shift in how we approach bone density. A groundbreaking April 2026 study published in the Journal of the American Heart Association (JAHA) has sent ripples through the medical community, revealing a concerning association between traditional calcium supplementation and the recurrence of major cardiovascular events.
As we move toward a more individualized era of medicine, the focus is shifting away from “piling on” mineral loads and toward optimizing the biological pathways that allow the body to manage its own calcium naturally. This is where Healobone—a non-calcium bone revival formula—is redefining the standard of care for fracture prevention and bone recovery.

The “Calcium Paradox”: Strengthening Bones or Stiffening Arteries?
The April 2026 JAHA study highlights what researchers call the “Calcium Paradox.” While the body needs calcium for skeletal structural integrity, high-dose supplemental calcium often fails to reach the bone matrix. Instead, it can settle in the soft tissues, most notably the arterial walls.
When calcium accumulates in the arteries, it leads to vascular calcification—a process that stiffens the vessels and significantly increases the risk of heart attacks and strokes. For patients already managing cardiovascular disease (CVD), the study found that calcium supplementation was linked to a higher rate of recurring cardiac events.
Why Traditional Calcium Supplements Often Fail:
- Poor Directed Transport: Without specific “signaling” nutrients, calcium remains in the bloodstream rather than entering the bone.
- Uptake Ceiling: The body can only process a limited amount of elemental calcium at once. Excess minerals are either excreted or deposited in the wrong places (kidney stones or arteries).
- Inflammation Gaps: Traditional minerals do not address the underlying inflammation that often drives bone loss in conditions like osteoporosis.
- Not combine with vitamin d3
- Absence of magnesium adequacy

Healobone: The Non-Calcium Strategy for Bone Revival
Healobone represents a departure from “mineral-heavy” formulas. Instead of adding more calcium to an already burdened system, Healobone provides the essential biological triggers that help your body utilize existing calcium more effectively while accelerating the natural repair of the bone matrix.
The Science Inside: Healobone’s Triple-Action Composition
Healobone’s effectiveness is rooted in its minimalist, evidence-based formulation:
1. Micronized Cissus Quadrangularis (500mg)
Often referred to as the “Bone Setter,” this phytochemical is clinically validated to:
- Accelerate Fracture Healing: It stimulates the metabolism and uptake of minerals by osteoblasts (bone-building cells).
- Reduce Pain and Inflammation: It acts as a natural analgesic, which is vital during post-fracture recovery.
- Osteoprotection: It helps maintain the balance between bone formation and resorption, making it ideal for osteopenia and osteoporosis management.
2. Liposomal Vitamin D3 (600 IU)
Not all Vitamin D is created equal. Healobone utilizes an Advanced Liposomal Delivery System.
- Superior Bioavailability: Liposomal encapsulation allows the D3 to bypass the harsh environment of the digestive tract, ensuring maximum absorption even in older adults with compromised gut health.
- The Key to Absorption: Vitamin D3 is the primary driver for intestinal calcium absorption, ensuring your body gets what it needs from your diet without needing high-dose pills.
3. Vitamin K2-7 (55mcg)
If Vitamin D3 is the “loader” that puts calcium into the blood, Vitamin K2-7 is the “Traffic Controller.”
- Directing Calcium: It activates Osteocalcin, a protein that binds calcium to the bone matrix.
- Cardiovascular Safety: Crucially, K2-7 prevents “ectopic calcification” by keeping calcium out of the arteries and heart valves, directly addressing the concerns raised in the recent JAHA publication.
Clinical Utility: Who Should Consider a Non-Calcium Approach?
1. The Osteoporosis & Osteopenia Patient
For those with thinning bones, the goal isn’t just “harder” bones, but “tougher” bones. Excess calcium can make bones brittle; Healobone focuses on the organic collagen matrix and osteoblast activity, improving bone quality and reducing fracture risk.
2. Post-Fracture Recovery
Fracture healing requires a massive surge in metabolic activity. Cissus Quadrangularis in Healobone has been shown in clinical settings to reduce healing time by up to 33%, allowing patients to return to mobility faster.
3. Orthopedic Surgery Support
Whether it is joint replacement or spinal fusion, the surrounding bone must be healthy enough to support implants. Healobone acts as a supportive therapy to ensure the structural “integration” of surgical sites.
4. Individuals at Cardiovascular Risk
As per the April 2026 research, patients with a history of heart disease, hypertension, or arterial stiffness should be extremely cautious with traditional calcium. Healobone provides a 100% calcium-free alternative that supports bones without endangering the heart.
For decades, calcium supplementation has been considered the foundation of osteoporosis prevention and fracture recovery protocols. However, a growing body of clinical evidence suggests that bone regeneration depends not only on calcium intake but also on how effectively calcium is absorbed, transported, and incorporated into skeletal tissue. This distinction is becoming increasingly important as clinicians reassess the long-term role of routine calcium supplementation in modern bone health strategies.
In April 2026, a large population-based cohort study published by the American Heart Association examined the association between calcium supplementation and recurrence of cardiovascular events in patients with established cardiovascular disease. The findings suggested a measurable relationship between routine calcium supplement use and increased risk of recurrent cardiovascular events in susceptible populations. While calcium remains essential in specific deficiency states, the study has prompted renewed discussion about whether traditional calcium-centered supplementation approaches should be reconsidered—particularly when safer regulatory micronutrient strategies may be available.
At the same time, the global burden of osteopenia, osteoporosis, osteosarcopenia, stress fractures, and avascular necrosis continues to rise despite widespread availability of calcium supplements. This paradox highlights an important clinical shift: improving bone repair today requires not simply increasing calcium intake, but restoring calcium homeostasis signaling through nutrients such as vitamin D3, magnesium, vitamin K2-7, and osteogenic botanical agents like Cissus quadrangularis, which support structural regeneration rather than mineral loading alone.
Calcium Supplementation vs Calcium Regulation Strategy in Modern Bone Care
Feature | Conventional Calcium Supplementation | Calcium Regulation–Focused Strategy |
Primary goal | Increase calcium intake | Improve calcium utilization and placement |
Depends on absorption efficiency | Yes | Less dependent due to signaling support |
Activates osteoblasts | Minimal | Yes (via vitamin D3, K2-7, Cissus quadrangularis) |
Prevents vascular calcium deposition | No | Supported by vitamin K2-7 |
Supports fracture healing speed | Limited | Enhanced through osteogenic signaling |
Improves microcirculation to bone | No | Supported indirectly via metabolic regulation |
Addresses osteosarcopenia | No | Yes (muscle–bone interaction support) |
Useful in AVN supportive care | Limited role | Potential supportive role |
Risk of soft tissue calcium deposition | Possible if excess intake | Reduced with regulatory approach |
Suitable for long-term metabolic bone health | Partial | Stronger integrative role |
Clinical Insight
Modern bone repair strategies increasingly emphasize calcium direction rather than calcium addition. Nutrients such as vitamin D3, magnesium, vitamin K2-7, and osteogenic botanical agents like Cissus quadrangularis help ensure that available calcium is efficiently incorporated into skeletal tissue instead of accumulating in vascular or soft tissues.
This regulatory approach is particularly relevant in patients with:
osteopenia despite supplementation
recurrent stress fractures
post-fracture delayed healing
steroid exposure
early avascular necrosis
metabolic bone fatigue
cardiovascular risk requiring cautious calcium use
Beyond Calcium: A Modern Strategy for Bone Repair, Osteoporosis, and Avascular Necrosis
For decades, calcium supplementation has been considered the cornerstone of bone health management. Yet globally—and particularly in India—the incidence of osteopenia, osteoporosis, osteosarcopenia, fragility fractures, and avascular necrosis (AVN) continues to rise. This paradox suggests that bone regeneration is far more complex than calcium replacement alone.
Emerging clinical thinking now emphasizes calcium utilization rather than calcium intake, shifting attention toward micronutrients that regulate bone remodeling, vascular supply, and osteoblast activation. A non-calcium–based strategy using agents such as Cissus quadrangularis, liposomal vitamin D3, and vitamin K2-7 represents a targeted approach aligned with contemporary bone biology.
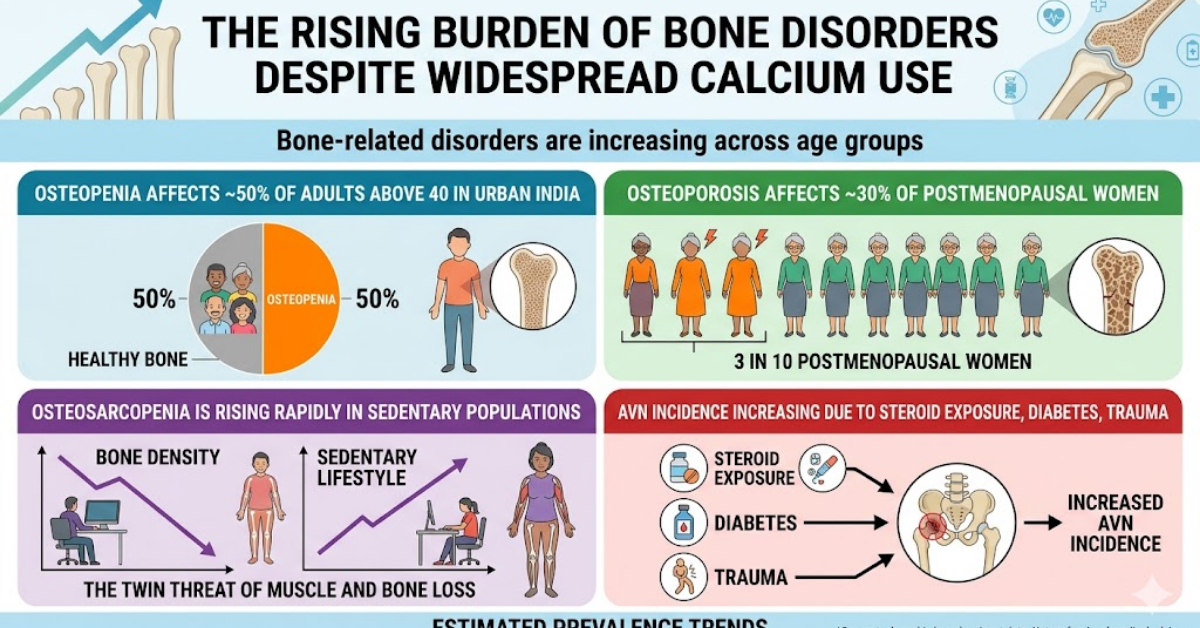
The Rising Burden of Bone Disorders Despite Widespread Calcium Use
Bone-related disorders are increasing across age groups:
Estimated prevalence trends:
Osteopenia affects ~50% of adults above 40 in urban India
Osteoporosis affects ~30% of postmenopausal women
Osteosarcopenia is rising rapidly in sedentary populations
AVN incidence increasing due to steroid exposure, diabetes, trauma
Fragility fractures projected to double globally by 2040
Despite widespread calcium supplementation, fracture rates continue to increase. This suggests the primary issue is not calcium deficiency alone—but impaired bone remodeling signaling.
Why Are Bone Problems Increasing Despite Calcium Supplementation?
Several biological limitations explain this trend:
Calcium absorption declines with age
Vitamin D insufficiency reduces calcium utilization
Magnesium deficiency impairs calcium transport
Vitamin K2 deficiency prevents calcium deposition in bone
Chronic inflammation inhibits osteoblast activity
Sedentary lifestyle reduces bone loading signals
Microvascular compromise reduces bone repair capacity
Bone regeneration depends on regulatory micronutrients, not calcium alone.
Recent Evidence: Cardiovascular Concerns with Calcium Supplementation
An April 2026 population-based cohort study published by the American Heart Association examined calcium supplementation in patients with cardiovascular disease and reported an association between calcium supplement use and increased recurrence of cardiovascular events in high-risk populations.
While calcium remains essential in selected clinical scenarios, this study reinforces growing concern that excess supplemental calcium—especially when poorly absorbed—may contribute to vascular calcification rather than skeletal benefit.
This finding strengthens interest in approaches that improve calcium directionality instead of calcium quantity.
Types of Calcium Supplements and Their Limitations
Calcium Type | Advantages | Limitations |
Calcium carbonate | High elemental calcium | Requires stomach acid, low absorption |
Calcium citrate | Better absorption | Lower elemental calcium |
Calcium lactate | Gentle on stomach | Requires frequent dosing |
Calcium gluconate | Mild | Low calcium content |
Coral calcium blends | Marketed as natural | Limited clinical superiority evidence |
Common limitations include:
- poor absorption
- constipation
- kidney stone risk
- vascular calcification risk
- dependency on vitamin D status
Calcium + Calcitriol Therapy: Benefits and Limitations
Calcium combined with calcitriol improves absorption and is frequently prescribed in osteoporosis and fracture care.
Benefits:
- enhances calcium uptake
- supports bone mineralization
- useful in elderly patients
Limitations:
- does not activate osteoblast signaling
- does not improve microcirculation
- does not prevent calcium misplacement
- may increase hypercalcemia risk with long-term use
Thus, it addresses availability but not utilization.
The Hidden Risk of Unabsorbed Calcium
Unabsorbed calcium may accumulate in:
- arterial walls
- kidneys
- soft tissues
Consequences include:
- vascular stiffness
- kidney stones
- calcific tendinopathy
Therefore, modern bone care increasingly focuses on calcium regulation pathways rather than supplementation alone.
Magnesium: The Missing Regulator of Bone Mineralization
Magnesium plays essential roles in:
- vitamin D activation
- parathyroid hormone signaling
- osteoblast stimulation
- calcium transport into bone matrix
Low magnesium reduces calcium incorporation efficiency.
Why Liposomal Magnesium Matters
Traditional magnesium salts:
- poor intestinal absorption
- dose-limited by diarrhea
- variable intracellular delivery
Liposomal magnesium:
- improves bioavailability
- enhances neuromuscular relaxation
- supports bone remodeling signaling
- improves vitamin D activation efficiency
Thus, magnesium delivery quality significantly influences skeletal outcomes.
Vitamin K2-7: The Calcium Traffic Controller
Vitamin K2-7 activates osteocalcin and matrix Gla-protein—two key regulators that direct calcium into bone and away from arteries.
Clinical roles:
- supports bone mineral density
- reduces vascular calcification
- enhances fracture healing signaling
- works synergistically with vitamin D3
Without K2-7, calcium cannot be efficiently deposited into skeletal tissue.
Cissus quadrangularis: A Traditional Agent with Modern Evidence
Cissus quadrangularis has been extensively studied for its osteogenic properties.
Mechanisms include:
- osteoblast activation
- collagen matrix stimulation
- bone mineralization acceleration
- anti-inflammatory activity
- analgesic effect in fracture pain
Studies show faster callus formation and earlier fracture union compared with controls.
Mechanism of Action
Component | Role |
Micronized Cissus quadrangularis | Stimulates osteoblast activity and fracture healing |
Liposomal Vitamin D3 | Improves calcium absorption and remodeling signaling |
Vitamin K2-7 | Directs calcium deposition into bone |
Together, these support structural repair rather than mineral loading alone.
Clinical Applications Across Bone Disorders
This strategy is applicable in:
- osteopenia
- osteoporosis
- post-fracture recovery
- stress fractures
- osteosarcopenia
- avascular necrosis support protocols
- chronic bone pain
- metabolic bone fatigue
Role in Avascular Necrosis (AVN)
AVN involves compromised blood supply and impaired bone remodeling.
Supportive micronutrient strategies aim to:
- improve osteoblast response
- enhance microvascular signaling
- reduce inflammation
- promote subchondral repair
Cissus quadrangularis has demonstrated promising osteogenic signaling effects in such contexts.
Pain Relief Benefits of Cissus quadrangularis
Unlike calcium supplements, Cissus provides:
- anti-inflammatory activity
- reduced fracture-site pain
- improved mobility
- earlier rehabilitation tolerance
This makes it useful in acute and chronic bone discomfort.
Safety Profile and Long-Term Use
Compared with high-dose calcium therapy:
- lower risk of vascular calcification
- lower kidney stone risk
- better gastrointestinal tolerance
- safe for extended use
This supports its suitability for long-duration skeletal repair programs.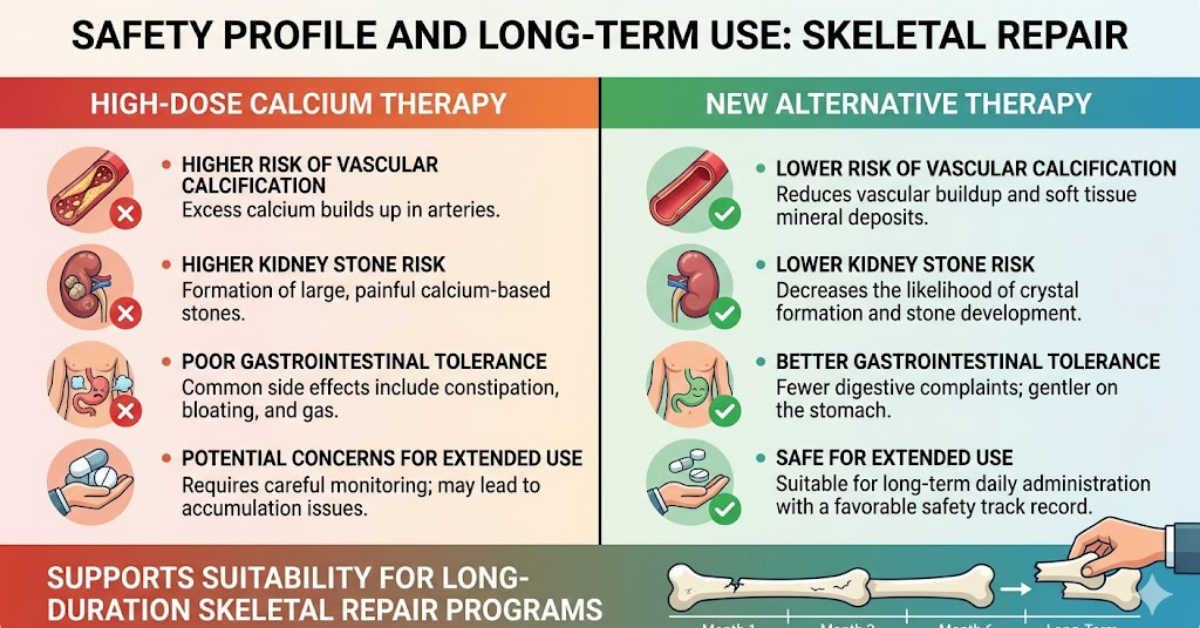
Comparison: Calcium-Centric vs Regulatory Bone Support Strategy
Feature | Calcium Supplements | Regulatory Bone Support |
Adds mineral | Yes | No |
Improves absorption signaling | Limited | Yes |
Directs calcium deposition | No | Yes |
Supports osteoblast activity | Minimal | Yes |
Reduces vascular calcification risk | No | Yes |
Supports fracture healing speed | Limited | Yes |
When Calcium Supplementation Is Still Needed
Calcium remains appropriate when:
- dietary calcium intake is low
- postmenopausal osteoporosis is severe
- chronic steroid therapy present
- documented hypocalcemia exists
However, regulatory micronutrients remain essential adjuncts.
Clinical Monitoring Strategy
Objective monitoring should include:
- vitamin D levels
- magnesium status
- bone density trends
- pain scores
- mobility improvement
- fracture healing timelines
Functional improvement should accompany laboratory correction.
Conclusion: A New Standard for Bone Care
The era of “more is better” for calcium is over. The latest scientific evidence demands a smarter, safer approach. By focusing on transport, signaling, and natural repair rather than mineral loading, Healobone offers a path to stronger bones and a healthier heart.
Disclaimer: This blog is for informational purposes and reflects recent scientific trends. Always consult with your healthcare provider or orthopedic specialist before starting a new supplement regimen, especially if you have pre-existing cardiovascular conditions.
References: Association Between Calcium Supplementation and Recurrence of Cardiovascular Events in Patients With Cardiovascular Disease: A Population‐Based Cohort Study, JAHA, April 2026.
Frequently Asked Questions
No. Healobone is a non-calcium bone formula. It is designed to help your body naturally manage and direct the calcium you already get from your diet or existing therapy.
Yes. Healobone is an ideal “companion therapy.” It provides the Vitamin K2-7 and D3 needed to ensure that your prescribed calcium actually reaches your bones instead of staying in your arteries.
Cissus is a powerful botanical known for its ability to increase bone-building cell activity and reduce inflammation. It is especially useful for accelerating the healing of micro-fractures and major breaks.
Yes. Liposomal delivery protects the vitamin as it passes through the stomach, leading to significantly higher absorption rates in the bloodstream compared to standard tablets.
Through its Vitamin K2-7 content, Healobone helps activate proteins that actively remove calcium from the arteries and move it into the bones, reducing the risk of vascular stiffness.
Yes. Unlike some NSAIDs or synthetic bone drugs, Healobone uses bio-available nutrients and botanicals that are safe for long-term support of bone health without gastric irritation.
Absolutely. Post-menopausal women are at the highest risk for bone loss (osteoporosis). Healobone helps counter this by stimulating osteoblast activity and improving calcium utilization during this critical life stage.
Yes. The Cissus Quadrangularis in Healobone has natural anti-inflammatory and analgesic properties that help manage discomfort during the healing process.
Recent studies, including the April 2026 JAHA report, indicate that excess supplemental calcium can contribute to heart disease by calcifying the arteries. A non-calcium strategy avoids this risk entirely.
The recommended dosage is typically one capsule daily or as directed by your healthcare professional. Each bottle contains a 30-day supply (30 capsules).