Chronic digestive issues in India are rising at an alarming rate. Whether it is persistent bloating after every meal, unpredictable bowel movements, or fatigue that never quite goes away — millions of Indians are living with symptoms they cannot explain. IBS symptoms in India have become so widespread that they are now one of the leading reasons for gastroenterology consultations across urban hospitals.
Yet despite how common these complaints are, there is enormous confusion about what is actually causing them. Three conditions — Irritable Bowel Syndrome (IBS), Small Intestinal Bacterial Overgrowth (SIBO), and Leaky Gut — are frequently mixed up, misdiagnosed, or treated interchangeably. Understanding the SIBO vs IBS difference, and where leaky gut fits in, is not just an academic exercise. It is the foundation of getting the right help.
Bloating causes and treatment options differ significantly depending on the underlying condition. Treating IBS with probiotics when the real driver is SIBO, for example, may provide temporary relief at best — and worsen symptoms at worst. This article breaks down each condition clearly, explains why they overlap, and outlines evidence-based, natural treatment for IBS and related gut disorders relevant to the Indian context.
Incidence & Relevance in India
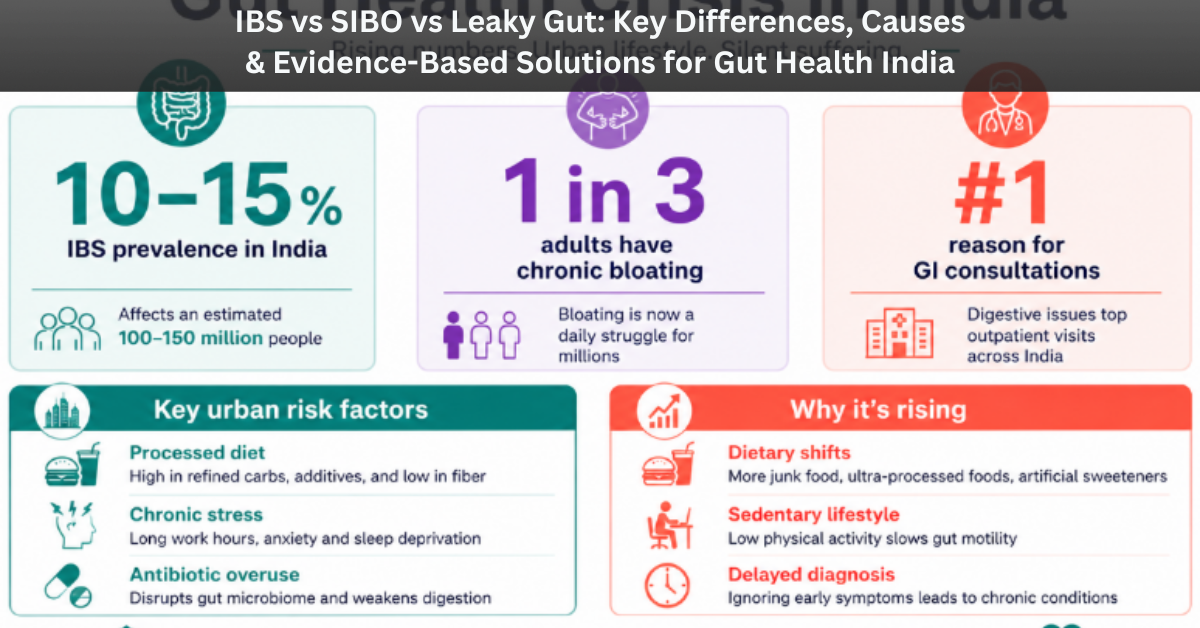
Gut health in India is under serious strain. IBS symptoms in India affect an estimated 10–15% of the population, with urban adults disproportionately affected. Rapid dietary shifts — away from traditional, fibre-rich Indian foods toward processed snacks, refined carbohydrates, and low-nutrient convenience meals — are significantly disrupting the gut microbiome.
Chronic digestive issues in India are compounded by three major lifestyle factors: high psychological stress, irregular sleep patterns, and widespread antibiotic overuse. India has one of the highest rates of antibiotic consumption globally, and repeated antibiotic courses are a well-established trigger for microbiome imbalance — a state in which harmful bacteria outcompete beneficial ones, setting the stage for conditions like SIBO and leaky gut.
The social stigma around discussing digestive symptoms openly means many people self-medicate for years before seeking proper diagnosis. By that point, what began as mild gut discomfort may have evolved into a complex, multi-layered condition requiring a more comprehensive approach. Gut health India deserves the same clinical attention as cardiovascular or metabolic health — and awareness is the first step.

What is IBS?
Irritable Bowel Syndrome is a functional gastrointestinal disorder — meaning there is no visible structural damage to the gut, yet the digestive system does not function normally. It is diagnosed based on a characteristic pattern of IBS symptoms in India and globally, using criteria known as the Rome IV diagnostic standards.
Common symptoms include recurring abdominal pain or cramping (often relieved after a bowel movement), alternating constipation and diarrhoea, persistent bloating, excess gas, and a sensation of incomplete evacuation. IBS is further classified into IBS-C (constipation-predominant), IBS-D (diarrhoea-predominant), and IBS-M (mixed type).
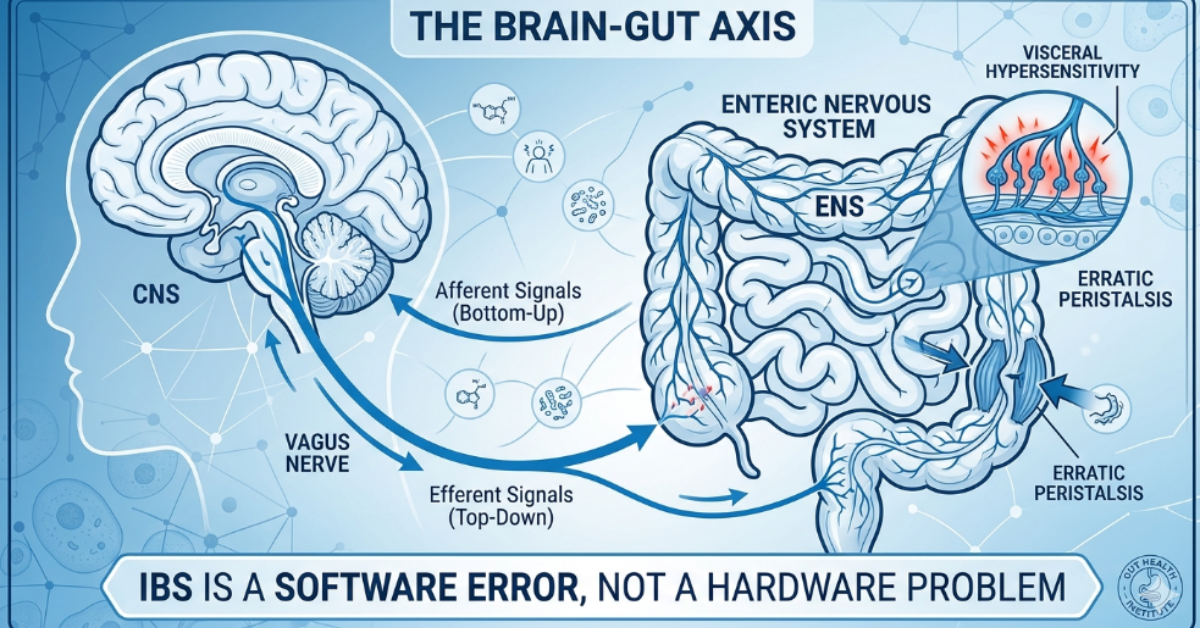
A defining feature of IBS is its strong connection to the brain-gut axis — the bidirectional communication network between the central nervous system and the enteric nervous system embedded in the gut wall. This explains why stress, anxiety, and emotional disturbances so reliably trigger or worsen IBS flares. Managing IBS without addressing psychological wellbeing is rarely effective long-term. Natural treatment for IBS almost always includes stress management as a core pillar, not an afterthought.
What is SIBO?
To understand the SIBO vs IBS difference, it helps to first understand what SIBO actually is. Small intestinal bacterial overgrowth (SIBO) occurs when bacteria that normally reside in the large intestine migrate into and colonise the small intestine in abnormally high numbers. The small intestine is naturally a low-bacteria environment; its primary role is nutrient absorption, not fermentation.
When this balance is disrupted, bacteria begin fermenting food in the small intestine — producing excess hydrogen or methane gas, interfering with nutrient absorption, and triggering a cascade of symptoms that closely mirror IBS. This is the crux of the SIBO vs IBS difference: IBS is a functional disorder with no known structural cause, while SIBO has a definable, testable bacterial overgrowth driving the symptoms.
SIBO develops through several pathways: poor gut motility that allows bacteria to accumulate, prior antibiotic use creating microbiome imbalance, low stomach acid (often from proton pump inhibitor overuse), or structural abnormalities in the gut. Research suggests that a significant proportion of IBS cases that do not respond to standard management may actually be driven by undetected SIBO — making accurate diagnosis critical. Bloating causes and treatment in SIBO require a fundamentally different approach than in straightforward IBS.
What is Leaky Gut?
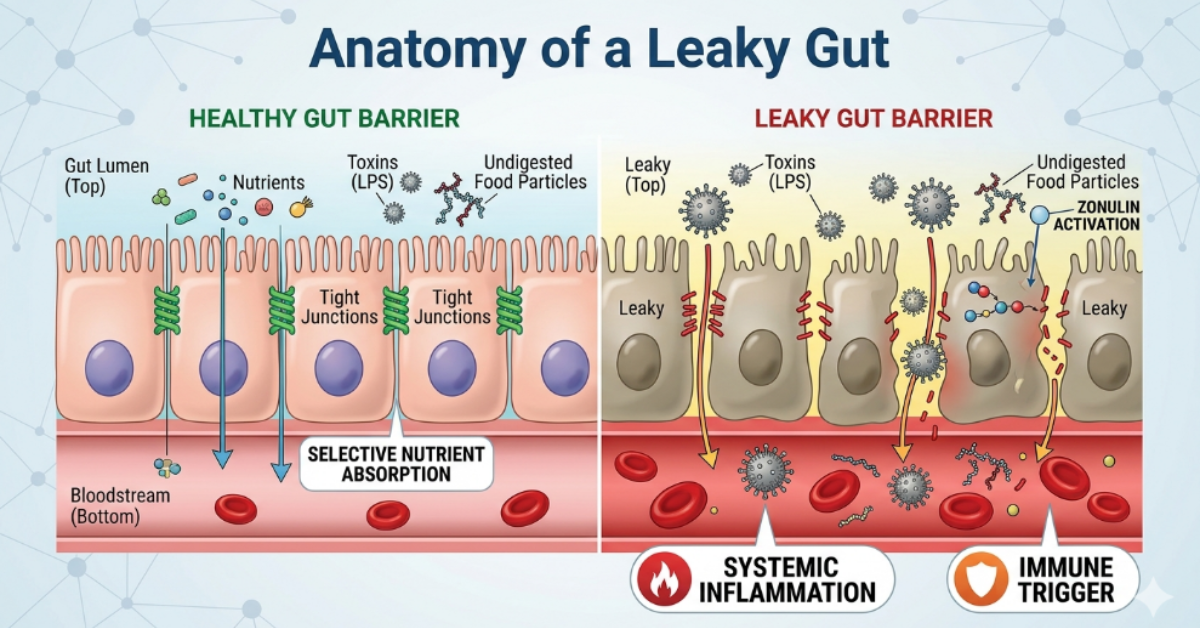
Leaky gut — clinically described as increased intestinal permeability — refers to a breakdown in the integrity of the gut lining. Under healthy conditions, the intestinal epithelium acts as a highly selective barrier: it allows nutrients to pass into the bloodstream while blocking harmful substances such as bacterial toxins, undigested food particles, and pathogens.
Leaky gut symptoms and causes are more varied and systemic than those of IBS or SIBO. When tight junctions between intestinal cells loosen, toxins and molecules that should remain in the gut enter systemic circulation, triggering widespread immune activation and inflammation. This is why leaky gut symptoms and causes extend far beyond the digestive tract — presenting as chronic fatigue, skin conditions like eczema, brain fog, joint pain, food sensitivities, and even autoimmune flares.
Intestinal permeability is increased by a range of factors: chronic dysbiosis (microbiome imbalance), a diet high in processed foods and alcohol, NSAID overuse, chronic psychological stress, and ongoing gut infections. Leaky gut is not yet classified as a standalone diagnosis in conventional medicine, but the evidence linking intestinal permeability to systemic inflammation is growing steadily. Addressing leaky gut is often essential to achieving lasting resolution of IBS and SIBO symptoms.
Feature | Irritable Bowel Syndrome (IBS) | Small Intestinal Bacterial Overgrowth (SIBO) | Leaky Gut (Permeability) |
Primary Issue | Functional / Communication | Bacterial Displacement | Structural / Barrier Breach |
Visible Damage | None (Functional) | None (Bacterial) | Tight Junction Breakdown |
Key Trigger | Stress, Anxiety, FODMAPs | Low Acid, Poor Motility | NSAIDs, Toxins, Dysbiosis |
Bloating Timing | Variable, often late day | Rapid (30-90 mins after eating) | Chronic, often with food reactions |
Diagnostic Test | Clinical History (Rome IV) | Breath Test (Hydrogen/Methane) | Zonulin Test / Lactulose-Mannitol |
Pain Source | Nerve Hypersensitivity | Gas Pressure in Small Bowel | Systemic Inflammatory Response |
Stool Changes | Strong correlation (D or C) | Common (often fatty stools) | Less specific to stool type |
Systemic Signs | Rare (mostly localized) | Weight loss, B12 deficiency | Fatigue, Rashes, Joint Pain |
Why IBS Comes and Goes
One of the most frustrating characteristics of IBS is its cyclical, unpredictable nature. Understanding why symptoms flare and remit is essential for long-term management.
Stress fluctuations are among the most reliable triggers. Cortisol and stress hormones directly alter gut motility, increase intestinal permeability, and shift microbiome composition. Periods of high personal or professional stress almost universally worsen IBS symptoms.
Diet plays an equally significant role. Fermentable carbohydrates (FODMAPs), caffeine, alcohol, and spicy foods act as direct irritants for many IBS sufferers. Since dietary habits vary day to day, symptoms naturally fluctuate in parallel.
Underlying SIBO cycles are a frequently overlooked explanation for why IBS comes and goes. If SIBO is an undiagnosed driver, symptoms may improve with dietary restriction as bacterial populations temporarily reduce — only to return as bacteria rebound. This pattern of improvement and relapse is a hallmark of untreated SIBO.
Hormonal changes, particularly in women, also drive IBS cyclicality. Oestrogen and progesterone significantly influence gut motility, and many women notice clear correlations between their menstrual cycle and digestive symptom intensity.
Finally, microbiome imbalance itself creates instability. A gut microbiome with low diversity is inherently more vulnerable to disruption. Any acute illness, antibiotic course, or dietary change can destabilise it further — triggering another symptom cycle.
Root Causes — an Integrated View
Rather than viewing IBS, SIBO, and leaky gut as entirely separate diseases, it is more clinically useful to see them as overlapping consequences of the same upstream disruptions:
Diet is foundational. Processed food consumption, excess refined sugar, low dietary fibre, and ultra-processed snacks deplete beneficial gut bacteria, promote dysbiosis, and increase intestinal permeability. The shift away from traditional Indian diets — rich in fibre, fermented foods, and whole grains — has been particularly damaging to gut health India-wide.
Chronic stress activates the HPA axis, suppresses immune tolerance, and creates the neurological conditions in which IBS thrives. Stress is not simply a trigger — it is a root cause.
Antibiotic overuse and NSAID dependency are two of the most direct pharmaceutical contributors to microbiome imbalance and gut lining damage respectively. Both are overused in India to a significant degree.
Poor gut motility — often a consequence of hypothyroidism, diabetes, post-infectious changes, or sedentary lifestyle — slows the intestinal cleansing wave (migrating motor complex), allowing bacteria to accumulate and SIBO to develop.
Chronic low-grade inflammation, once established, becomes self-sustaining — perpetuating dysbiosis, worsening barrier function, and amplifying symptom cycles across all three conditions.
Preventive & Lifestyle Approach
Addressing chronic digestive issues in India requires a multi-pronged lifestyle approach, not just symptom suppression.
On the dietary front, the low-FODMAP diet is the most evidence-based intervention for reducing bloating causes and treatment of IBS and SIBO-related symptoms. It temporarily eliminates fermentable carbohydrates that feed gut bacteria, providing symptomatic relief while the root cause is addressed. It is best used as a short-term diagnostic and relief tool (4–8 weeks) under dietitian supervision, as long-term restriction reduces microbiome diversity.
An anti-inflammatory diet — emphasising colourful vegetables, whole grains, healthy fats such as olive oil and moderate ghee, lean proteins, and anti-inflammatory spices — supports gut lining repair and reduces systemic inflammation. Turmeric, ginger, and fenugreek, all staples of traditional Indian cooking, have genuine evidence behind their gut-protective properties.
Fibre balance matters. Soluble fibre — from oats, psyllium husk, and bananas — is generally better tolerated in IBS and SIBO than insoluble fibre. Introduce increases gradually to avoid exacerbating gas.
For lifestyle, stress management through yoga, pranayama, and mindfulness meditation directly modulates the brain-gut axis and has demonstrated measurable benefit in IBS clinical trials. Sleep quality is equally important — disrupted circadian rhythm dysregulates the gut microbiome and increases intestinal permeability. Prioritising 7–8 hours of restorative sleep is not optional in gut health recovery. Regular moderate physical activity improves gut motility, reduces cortisol, and supports microbiome diversity.
Evidence-Based Botanicals & Nutraceuticals
When lifestyle modifications alone are insufficient, targeted nutraceuticals may provide meaningful additional support as part of a structured management plan. The following ingredients have a credible evidence base for gut health India and globally.
Curcumin for gut health is one of the most extensively researched natural interventions available. The primary bioactive of turmeric, curcumin has demonstrated consistent anti-inflammatory effects in gut mucosa through inhibition of the NF-κB signalling pathway. It may support intestinal barrier integrity and reduce the inflammatory burden underlying IBS and leaky gut. Standard curcumin suffers from extremely poor bioavailability; micellar and phospholipid-bound formulations overcome this limitation significantly.
Probiotics India-wide are increasingly recognised as an important tool for microbiome imbalance correction. Multi-strain formulations containing Lactobacillus and Bifidobacterium species have demonstrated consistent benefit in IBS management — reducing bloating, improving stool consistency, and modulating the gut immune environment. Choosing a well-characterised, clinically studied formulation is essential.
Prebiotics such as fructooligosaccharides (FOS) and partially hydrolysed guar gum serve as selective fuel for beneficial gut bacteria, supporting long-term microbiome balance. They should be introduced carefully in active SIBO cases, as fermentation in the small intestine can temporarily worsen symptoms.
Herbal antimicrobials including berberine, oregano oil, and allicin show evidence of reducing small intestinal bacterial load — making them relevant to SIBO management as part of a clinician-guided protocol.
Gut barrier support nutrients — zinc, L-glutamine, and Vitamin D — are essential cofactors for intestinal tight junction protein expression, supporting repair of increased intestinal permeability over time.
Mechanism of Action
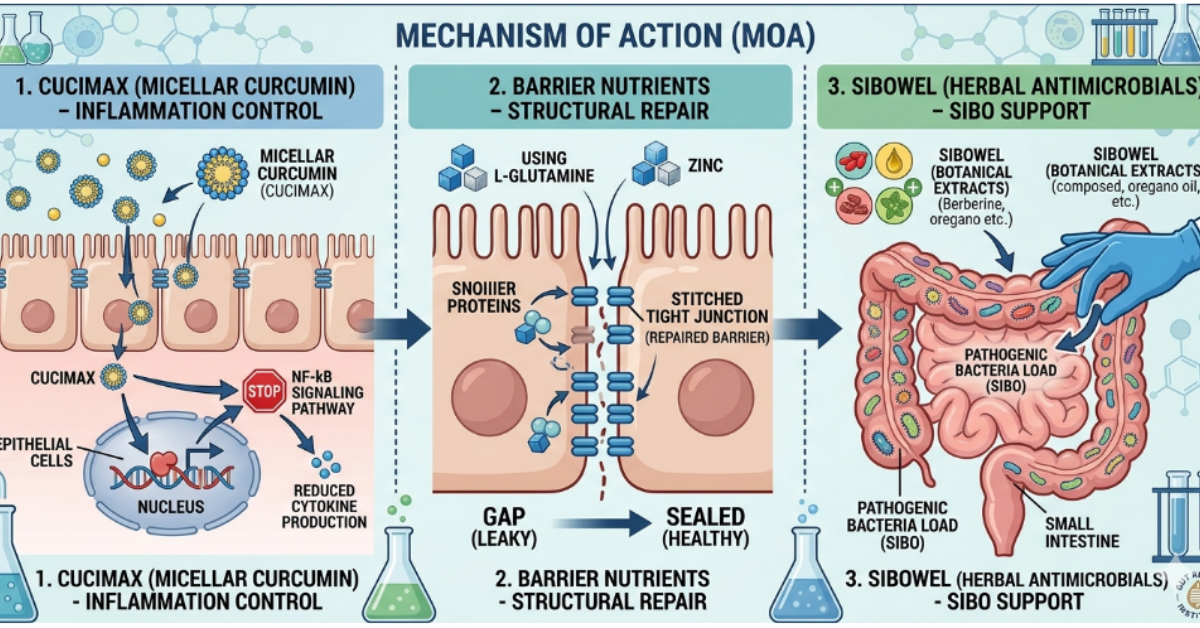
Understanding how these ingredients work adds important clinical credibility:
Curcumin for gut health operates primarily through NF-κB inhibition — blocking the nuclear factor kappa-B transcription pathway that drives production of pro-inflammatory cytokines including IL-1β and TNF-α in the gut mucosa. It also supports the expression of tight junction proteins, directly addressing leaky gut at a molecular level.
Probiotics restore microbiota diversity through competitive colonisation, crowding out pathogenic bacteria and communicating with mucosal immune cells (Peyer’s patches) to downregulate inappropriate inflammatory responses.
Herbal antimicrobials demonstrate direct activity against both gram-positive and gram-negative bacteria in the small intestine, reducing the bacterial load that drives SIBO symptoms — without the broad collateral disruption associated with conventional antibiotics.
Barrier nutrients, particularly zinc and L-glutamine, are prerequisites for intestinal epithelial cell proliferation and the synthesis of claudin, occludin, and ZO-1 — the tight junction proteins that determine intestinal permeability.
Evidence-Based Product Options
The following products are designed to address specific aspects of gut dysfunction and may support symptom management as part of a broader, clinician-guided plan:
CUCIMAX (Micellar Curcumin) utilises micellar nanotechnology to dramatically improve curcumin bioavailability compared to standard preparations. This makes curcumin for gut health genuinely effective at the mucosal level — supporting inflammation control and intestinal barrier integrity. Best used as part of a structured anti-inflammatory protocol.
PRIZIBIOM / PRIZIBIOM LITE are formulated to support gut microbiome diversity and digestive balance. Containing carefully selected probiotic strains relevant to probiotics India research, these products may help restore healthy bacterial populations disrupted by diet, stress, or antibiotic use. PRIZIBIOM LITE offers a gentler entry point for sensitive individuals.
SIBOWEL is specifically formulated to target bacterial imbalance in the gut, combining herbal antimicrobial botanicals with gut-supportive nutrients. It can support management of SIBO-related symptoms as part of a structured, clinician-supervised plan — addressing one of the most underrecognised drivers of chronic bloating causes and treatment failure in IBS.
PRIZBIOM LITE: A gentle, beginner-friendly synbiotic (probiotic + prebiotic) formula specifically designed for sensitive stomachs. It is ideal for daily use to manage mild bloating, gas, and discomfort while improving gut barrier integrity. The inclusion of L-Glutamine provides essential structural support for repairing the gut lining.
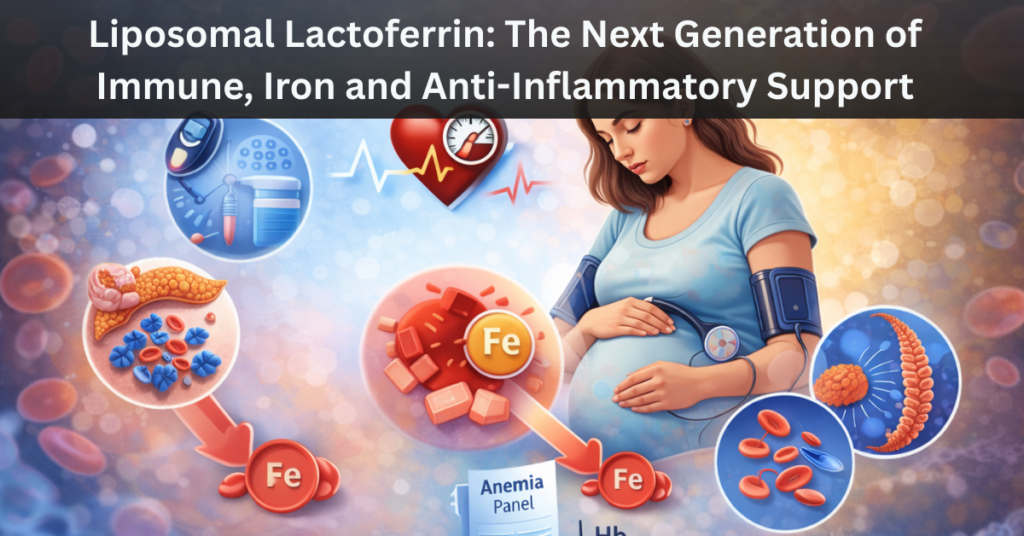
LF-MAX (Liposomal Lactoferrin): An advanced formula designed to support infection management, immune resilience, and efficient iron utilization in cases of anemia. Its liposomal delivery ensures superior cellular uptake and absorption. Beyond immunity, lactoferrin promotes the growth of beneficial gut bacteria while inhibiting harmful pathogens, making it highly relevant for those with IBS or microbiome imbalances.
All supplementation decisions should be made in consultation with a qualified healthcare professional. These products can support — but not replace — dietary and lifestyle interventions.
Benefits of Evidence-Based Supplementation
Targeted support means ingredients are chosen for their specific mechanisms — gut inflammation, barrier repair, or microbial balance — rather than generic wellness claims. This precision matters when conditions like IBS, SIBO, and leaky gut each require a different biochemical approach.
Faster symptomatic relief alongside dietary changes may reduce the duration and intensity of flares, improving quality of life during the recovery phase. Better compliance follows from well-tolerated, clearly dosed formulations that fit into daily routines without complexity. Scientific backing distinguishes evidence-based nutraceuticals from wellness trends — ingredients supported by peer-reviewed clinical research, not just traditional claims or marketing. Finally, compatibility with conventional care means these supplements can be integrated alongside gastroenterologist-guided management, creating a more comprehensive approach than either alone.
Frequently Asked Questions
IBS is a chronic functional condition that can be effectively managed rather than permanently cured in the conventional sense. Many people achieve long-term remission and extended symptom-free periods with the right dietary, lifestyle, and supplementation approach. Addressing underlying drivers such as microbiome imbalance or SIBO often leads to significant and lasting improvement in IBS symptoms in India and globally.
The gold-standard test is the hydrogen and methane breath test. After consuming a lactulose or glucose solution, gas levels in your breath are measured over 1–3 hours. Elevated hydrogen or methane indicates bacterial fermentation occurring in the small intestine. A gastroenterologist can arrange this investigation.
The gut lining has a remarkable capacity for self-repair. With removal of dietary triggers (alcohol, processed foods, gluten in sensitive individuals), consistent stress reduction, adequate sleep, and targeted nutritional support including zinc, L-glutamine, and probiotics, intestinal permeability can normalise meaningfully over weeks to months.
Yes. LF-MAX supports iron utilization, which is often compromised in chronic gut conditions, potentially improving energy levels while simultaneously supporting your immune system’s management of gut pathogens.
PRIZBIOM LITE is specifically designed as a “beginner-friendly” synbiotic for sensitive individuals. It focuses on gentle microbiome support and includes L-Glutamine to help soothe and repair the gut lining.
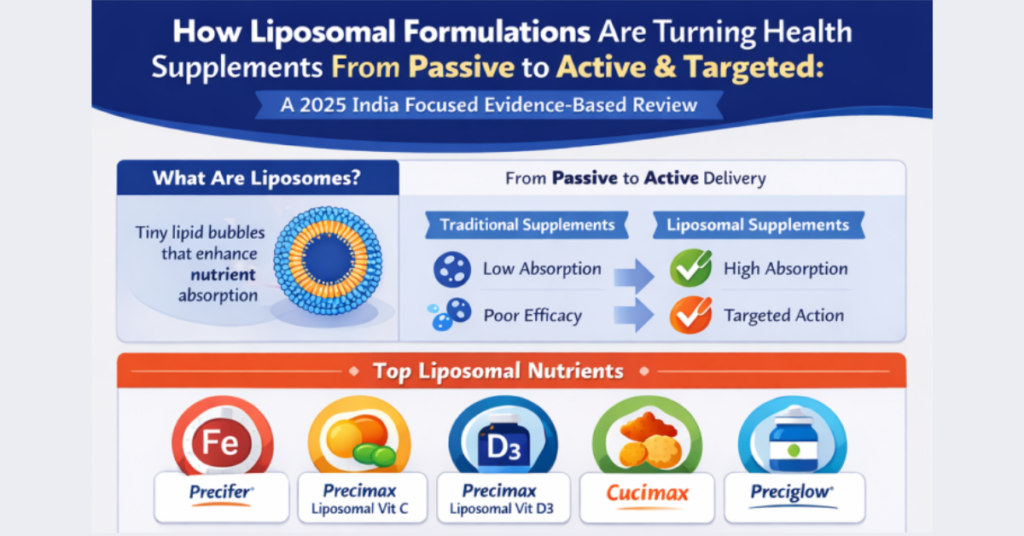
Standard supplements often have poor absorption. Micellar (like in CUCIMAX) and Liposomal (like in LF-MAX) technologies wrap the active ingredients in fats that the body absorbs more easily, ensuring the nutrients actually reach your cells and gut mucosa.
While probiotics add “good” bacteria, SIBOWEL contains herbal antimicrobials designed to reduce the “overgrowth” of bacteria in the small intestine, addressing the root cause of SIBO-related bloating.
IBS-C is constipation-predominant IBS, IBS-D is diarrhoea-predominant, and IBS-M is mixed type. These subtypes respond differently to dietary and nutraceutical interventions, making subtype identification an important early step in management.
Clinical evidence consistently supports curcumin for gut health, particularly its ability to inhibit NF-κB — a central driver of mucosal inflammation. Enhanced delivery formulations such as micellar curcumin are preferred, as standard curcumin has very poor bioavailability and may not achieve meaningful gut-level concentrations.
The SIBO vs IBS difference is not reliably identifiable through symptoms alone due to their significant overlap. Accurate diagnosis requires clinical assessment and, in SIBO’s case, a breath test. Treating SIBO as if it were simple IBS results in prolonged suffering and missed root-cause management.
They are closely related but distinct. Leaky gut can cause or significantly worsen food intolerances by allowing partially digested food proteins to trigger immune reactions in the bloodstream. Resolving increased intestinal permeability over time may reduce the number and severity of food intolerances.
Mild microbiome imbalance may improve within 4–8 weeks of dietary changes and probiotic use. Established SIBO or significant intestinal permeability may require 3–6 months of consistent, structured intervention. Identifying and addressing the root cause — rather than only managing symptoms — is the most important determinant of recovery speed.
Phytoceuticalantimicrobials show comparable SIBO treatment efficacy to rifaximin in some studies, with a generally narrower disruption profile. However, they should still be used under clinical guidance, as inappropriate use can alter microbiome balance in unintended ways.
Yes, both conditions occur in children, though they are more commonly discussed in adults. Childhood IBS is frequently linked to anxiety, dietary patterns, and post-infectious gut changes. A paediatric gastroenterologist should be involved in any diagnostic and management decisions.
The brain-gut connection is bidirectional and well-established. Anxiety and depression are significantly more prevalent in people with IBS. Treating gut issues often improves mental wellbeing, and addressing mental health reliably reduces gut symptom severity. An integrated approach remains the most effective strategy.
Sleep deprivation disrupts the circadian rhythm of the gut microbiome, reduces beneficial bacterial populations, increases intestinal permeability, and heightens visceral pain sensitivity. Consistent, restorative sleep is one of the most underappreciated pillars of gut health India practitioners are beginning to emphasise more strongly.
Common triggers include maida (refined flour), deep-fried snacks, rajma and chhole (high-FODMAP legumes in large quantities), excess chai and coffee, and heavily spiced curries. A dietitian-supervised low-FODMAP approach can help identify individual triggers within the context of an Indian dietary pattern.
SIBO is increasingly recognised in India, particularly among those with a history of antibiotic overuse, proton pump inhibitor use, or recurrent gut infections. It remains significantly underdiagnosed due to limited breath test availability outside major metropolitan centres and low clinical awareness at the primary care level.
Yes. Chronic IBS is associated with low-grade mucosal inflammation that can progressively compromise the intestinal barrier, contributing to increased intestinal permeability. Conversely, leaky gut worsens IBS symptoms — creating a reinforcing cycle that requires addressing both conditions simultaneously for meaningful resolution.
Strains with the strongest IBS evidence include Lactobacillus rhamnosus GG, Bifidobacterium infantis, and Lactobacillus plantarum. Multi-strain probiotics India formulations combining several of these have shown consistent benefit in clinical trials. Always choose products with documented CFU counts, strain-level identification, and appropriate storage conditions.